Study Design And Procedure
Primary objective of this study is to evaluate whether Overactive Bladder Symptoms Score of female patients with latent FC is higher than that of patients without latent FC at the urological department of the general hospital or not. For the secondary objectives are to investigate the associated factors for latent FC and mild to moderate OAB, wet OAB, and dry OAB. Sample size was determined by the free software of Vanderbilt University.
Urinary symptoms were evaluated by OABSS and constipation was evaluated by the Rome III criteria. The OABSS was developed to assess the presence and severity of OAB symptoms as a self-administered four-item questionnaire . OAB was defined as OABSS 3 and Q3 2 and it was classified into wet OAB, which was OAB with urinary incontinence, and dry OAB, which was OAB without urinary incontinence. OAB was also classified into three severity categories as follows: mild OAB , moderate OAB , and severe OAB . The Rome III criteria include six items related to defecation: straining, lumpy hard stools, sensation of incomplete evacuation, use of digital maneuvers, sensation of anorectal obstruction or blockage with 25 percent of bowel movements, and decrease in stool frequency . Latent FC was defined by positivity for two or more of the Rome III criteria . The clinical background was also investigated, including the medical history and drug therapy .
Caffeinated Foods And Drinks
As a diuretic, caffeine may aggravate symptoms associated with urinary retention, such as urgency. Caffeine occurs in a variety of different foods, including chocolate, coffee and tea. NAFC reports that limiting your intake of caffeine to 100 milligrams a day may reduce symptoms. For reference, 1 cup of coffee has 135 milligrams to 200 milligrams of caffeine, 1 cup of tea has 15 milligrams to 50 milligrams and one piece of sweet chocolate has 19 milligrams.
Constipation And The Bowel
Severe constipation is the most common cause of faecal incontinence , especially in older people. This is because hard bowel motions are difficult to pass and may cause a partial blockage high up the bowel, resulting in watery bowel motions flowing around the constipated stool without warning. This is sometimes mistaken for diarrhoea.
You can use the Bristol Stool Chart to check what your bowel motions should look like.
Don’t Miss: How To Help Heartburn Fast
Symptoms Of A Urinary Tract Infection
Symptoms of a lower UTI include
- Pain or discomfort when urinating
- The feeling of being unable to empty your bladder fully
- Cloudy and/or foul-smelling urine that may contain blood
- Pain in your lower abdomen and pelvis
- Feeling achy, tired and generally under-the-weather
Symptoms of an upper UTI include
- A high temperature of 38°C
- Pain in your sides or back
- Shivering or chills
- Agitation or restlessness
Initial Management Of Urinary Retention
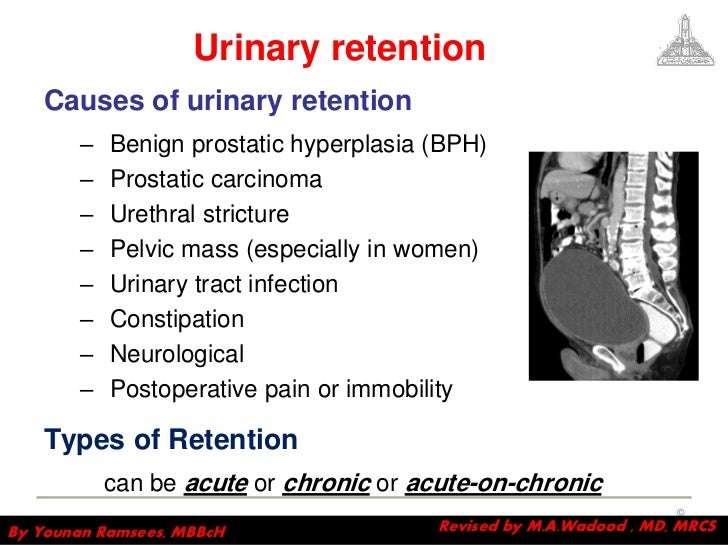
Acute urinary retention should be managed by immediate and complete decompression of the bladder through catheterization. Standard transurethral catheters are readily available and can usually be easily inserted. If urethral catheterization is unsuccessful or contraindicated, the patient should be referred immediately to a physician trained in advanced catheterization techniques, such as placement of a firm, angulated Coude catheter or a suprapubic catheter.5 Hematuria, hypotension, and postobstructive diuresis are potential complications of rapid decompression however, there is no evidence that gradual bladder decompression will decrease these complications. Rapid and complete emptying of the bladder is therefore recommended.34
For hospitalized patients requiring catheterization for 14 days or less, a Cochrane review found that silver alloy-impregnated urethral catheters have been associated with decreased rates of UTI versus standard catheters.41 Another Cochrane review concluded that patients requiring catheterization for up to 14 days had less discomfort, bacteriuria, and need for recatheterization when suprapubic catheters were used compared with urethral catheters.42 In a recent meta-analysis of abdominal surgery patients, suprapubic catheters were found to decrease bacteriuria and discomfort and were preferred by patients.43 Although evidence suggests short-term benefit from silver alloy-impregnated and suprapubic catheters, their use remains somewhat controversial.
You May Like: How To Get Rid Of Protein Bloat
What Are The Complications Of Urinary Retention
Complications may include:
- Urinary tract infection . When urine stays in the bladder, bacteria can grow and infect the urinary tract.
- Bladder damage. If the bladder becomes stretched too far or for long periods of time, the muscle may be permanently damaged and lose its ability to contract.
- Chronic kidney disease. If urine backs up into the kidneys it can lead to permanent kidney damage, reduced kidney function and chronic kidney disease.
Recognizing A Chronic Problem
So, how can you recognize chronic constipation and put an end to it before it causes your child even more discomfort? Know the symptoms.
The most common symptoms of chronic constipation include:
- Changes in appetite, including your child suddenly becoming full very easily
- Constant or frequent abdominal pain and cramps
- Irritability
- Nausea and vomiting
- Urinary problems as a result of an enlarged rectum leaving less room for the bladder to expand this means your child will need to urinate more frequently and they may get urinary tract infections or bladder infections
If you notice these changes in your childs bathroom habits and overall attitude and behavior, it is time to call the pediatrician. Your doctor will be able to set you and your child on the right path and will come up with a treatment plan based on your kids symptoms.
Constipation, even if it is chronic, is usually easily resolvable, and your doctor may prescribe certain laxatives or stool softeners to make your childs return to normal a little bit easier. Your doctor will likely also advise you to keep your child on a high fiber diet for a period of time since fiber helps keep things moving along through the digestive system. In fact, insufficient fiber may have been what caused the problem in the first place.
Also Check: Does Pasta Make You Bloated
Why Do Bladder And Bowel Incontinence Happen
When the bladder and bowel function normally, nerves tell certain muscles when to tense up and when to relax. Nerves in the spinal cord send messages from the brain to the bladder. Sphincter muscles control the flow of urine. Muscles in the rectum and anus control or release stool. These nerve and muscle processes allow urine and feces to be removed when you want them to.
Foods That Aggravate Urinary Retention
Not being able to fully relieve your bladder is not only uncomfortable but can also be dangerous, according to the National Institute of Diabetes and Digestive and Kidney Diseases. While no direct connection exists between diet and urinary retention, certain foods may aggravate your bladder. Consult your doctor to discuss how diet might affect your health when it comes to bladder control.
Read Also: Why Does My Stomach Feel Tight And Bloated
What Are The Complications Of Urinary Retention And Its Treatments
- Urinary tract infections : Because urine is normally sterile and the normal flow of urine usually prevents bacteria from infecting the urinary tract, developing urinary retention means an abnormal urine flow gives bacteria at the opening of the urethra a chance to infect the urinary tract.
- Bladder damage: If your bladder is stretched too far or for extended periods, the muscles may become permanently damaged and lose their ability to properly contract.
- Kidney damage: Sometime urinary retention can cause urine to flow back into the kidneys. This is called reflux and can damage or scar the kidneys.
- Urinary incontinence : Transurethral surgery to treat an enlarged prostate can result in urinary incontinence in some men. Its often temporary with most men gaining bladder control in a few weeks or months after surgery. The removal of tumors or cancerous tissue in the bladder, prostate, or urethra may also result in urinary incontinence.
The Link Between Urinary Incontinence And Constipation
Do you have urinary incontinence? Do you struggle with having regular bowel movements and feel constipated? Do you sometimes think when you struggle with bowel movement that your urinary leakage is worse?
Urinary incontinence can be caused by many factors, with one of the main contributors being constipation. Constipation is when someone passes less than 3 bowel movements per week or has difficulty with bowel movements. Constipation is discussed very frequently with patients because the enlarged colon places more pressure onto the bladder, which can make incontinence and urgency worse. There are several ways to help constipation. Lets talk about one of those ways- adjusting how you sit while you have a bowel movement.
Unfortunately, our toilets are not designed to help us have easy bowel movements. Instead, they actually cause our puborectalis muscle to tense. This muscle slings around the rectum, and its job is to keep stool in, but it also needs to be able to relax to let stool out.
So what can you do to help relax that muscle, thus helping you to have easier bowel movements? Sitting with your feet propped on a foot stool brings your knees slightly above your hips, which then places the puborectalis muscle in a lengthened position and allows for less tension on the rectum.
Don’t Miss: How Early In Pregnancy Can You Get Heartburn
Causes Of Total Incontinence
Total incontinence is when your bladder cannot store any urine at all. It can mean you either pass large amounts of urine constantly, or you pass urine occasionally with frequent leaking in between.
Total incontinence can be caused by:
- a problem with your bladder from birth
- injury to your spinal cord this can disrupt the nerve signals between your brain and your bladder
- a bladder fistula a small, tunnel like hole that can form between the bladder and a nearby area, such as the vagina
Dietary Tips For Managing Constipation
Try to drink at least 4-6 glasses of fluid a day and increase your fibre intake from a wide variety of foods. Fibre is classified as either soluble or insoluble. Most plant foods contain a combination of both types of fibre. Insoluble fibre such as wheat bran, wholegrain breads and cereal helps increase the dry weight and ability of bowel motions to hold moisture. Soluble fibre such as in fruits, vegetables and legumes help to soften the poo and make it easier to pass.
Processed foods such as biscuits, cakes, pastries and fast foods are generally low in fibre and will contribute to constipation. Fruit and vegetable juice contain little fibre and are not a good substitute for whole fruit and vegetables.
Don’t Miss: Does Heating Pad Help Bloating
Causes Of Stress Incontinence
Stress incontinence is when the pressure inside your bladder as it fills with urine becomes greater than the strength of your urethra to stay closed. Your urethra is the tube that urine passes through to leave the body.
Any sudden extra pressure on your bladder, such as laughing or sneezing, can cause urine to leak out of your urethra if you have stress incontinence.
Your urethra may not be able to stay closed if the muscles in your pelvis are weak or damaged, or if your urethral sphincter the ring of muscle that keeps the urethra closed is damaged.
Problems with these muscles may be caused by:
- damage during childbirth particularly if your baby was born vaginally, rather than by caesarean section
- increased pressure on your tummy for example, because you are pregnant or obese
- damage to the bladder or nearby area during surgery such as the removal of the womb , or removal of the prostate gland
- neurological conditions that affect the brain and spinal cord, such as Parkinson’s disease or multiple sclerosis
- certain connective tissue disorders such as Ehlers-Danlos syndrome
- certain medicines
How Does Irritable Bowel Syndrome Affect The Digestive System
Irritable bowel syndrome is a prevalent condition affecting the large intestine. Cramping, stomach discomfort, bloating, gas, diarrhea, constipation, or both are signs and symptoms. IBS is a chronic ailment that requires long-term management. It is diagnosed by looking at its clinical features along with the results of testing your stool for fat, blood, and other substances.
The two main types of IBS are constipation-predominant IBS and diarrhea-predominant IBS. With these diagnoses, you can then also specifically identify the type of irritable bowel syndrome you have. Constipation-predominant IBS is more common in women, while diarrhea-predominant IBS affects men more often than not.
Both types of IBS involve recurrent abdominal pain and changes to the frequency of stools. This can lead to problems with digestion as well as anxiety and depression if not treated properly. The only way to confirm an IBS diagnosis is through examination of your gut tissue and/or feces. This would reveal any underlying causes for your symptoms.
Treatment for IBS varies depending on what type of IBS you have. There are many different options available, such as dietary changes, medications, exercise, and self-help techniques. Your doctor will help you determine the best course of action based on your situation.
Recommended Reading: Does Lactose Intolerance Cause Constipation
How Long Can A Bout Of Irritable Bowel Syndrome Last
Irritable bowel syndrome is a prevalent digestive illness that affects many people. It causes stomach pains, bloating, diarrhea, and constipation among other symptoms. These tend to come and go throughout time, lasting days, weeks, or months at a time. It is frequently a lifetime issue. However, the periods of irritability are usually quite shortâno longer than two years.
It is difficult to say how long IBS symptoms will continue once they start. They may be temporary or permanent. Temporary symptoms include cramping, pain, and diarrhea. When you first develop IBS, these symptoms are likely to last only for a few days. Over time, however, they may last for more than two weeks. This is called chronic irritable bowel syndrome .
The severity of your symptoms may also change over time. For example, you may initially experience diarrhea as your main symptom. But if the cause of your diarrhea is found , then treatment should be focused on removing the cause, and not all patients will need medication for this condition. If the problem is resolved, then your diarrhea should resolve too.
Some patients with IBS may experience intermittent symptoms. These patients will sometimes feel fine and not experience any problems of their own, but occasionally the absence of symptoms is not enough for some people. If this is you, then one day you wake up and find yourself in severe pain or having diarrhea.
Treatment From A Gp For Utis That Keep Coming Back
If your UTI comes back after treatment, you may have a urine test and be prescribed different antibiotics.
Your doctor or nurse will also offer advice on how to prevent UTIs.
If you keep getting UTIs and regularly need treatment, a GP may give you a repeat prescription for antibiotics.
If you have been through the menopause, you may be offered a vaginal cream containing oestrogen.
Recommended Reading: Cystex Urinary Pain Relief Side Effects
Also Check: How To Keep Gut Microbiome Healthy
Causes Of Urge Incontinence
The urgent and frequent need to pass urine can be caused by a problem with the detrusor muscles in the walls of your bladder.
The detrusor muscles relax to allow the bladder to fill with urine, then contract when you go to the toilet to let the urine out.
Sometimes the detrusor muscles contract too often, creating an urgent need to go to the toilet. This is known as having an overactive bladder.
The reason your detrusor muscles contract too often may not be clear, but possible causes include:
- drinking too much alcohol or caffeine
- not drinking enough fluids this can cause strong, concentrated urine to collect in your bladder, which can irritate the bladder and cause symptoms of overactivity
Overflow incontinence may also be caused by your detrusor muscles not fully contracting, which means your bladder does not completely empty when you urinate. As a result, the bladder becomes stretched.
Your detrusor muscles may not fully contract if:
- there’s damage to your nerves for example, as a result of surgery to part of your bowel or a spinal cord injury
- you’re taking certain medicines
Avoid Constipation For The Bladder
You should try and avoid being constipated as this can bring on other symptoms and problems. For example, when the bowel does not empty properly it will swell up and push down onto the bladder and could cause urinary problems.
You can avoid constipation by following a healthy diet, which can also help some bladder problems. A good diet will not only benefit your bladder but also your health in general. Try and eat a balanced diet that is not too high in fat and includes plenty of fibre. Aim for at least five portions of fruit and vegetables a day. Choose wholegrain varieties of bread, pasta and rice, rather than white versions.
Being overweight can also make your bladder problems worse. Extra weight may put pressure on the pelvic floor muscles which can become weak.
Read Also: What Do You Do When You Have Diarrhea
Enhancing Healthcare Team Outcomes
The health outcomes can be enhanced by a thorough history using the questions suggested by the American Urological Association. One needs to obtain a medication review and perform a thorough physical examination to rule out a neurological disorder. Patients should receive counseling about catheter care and the importance of antisepsis. The nursing team needs to know of contraindications of catheter placement and be able to recognize them. Timely, urologic consultation for suprapubic catheterization is the recommendation in patients who have acute retention and inability to pass a urethral catheter. The clinician needs to be knowledgeable of how to do suprapubic needle drainage or temporary catheter drainage if the patient is in extreme discomfort or distress when a urologist is not immediately available.
The patient and patients support should receive training regarding clean intermittent catheterization, as well as education on medications used to treat benign prostatic hyperplasia.
Coordination between primary care clinicians, nephrologists, urologists, and emergency room clinicians is needed. Urology nurses educate patients, monitor their condition and provide update information to the interprofessional team. Pharmacists assess medications, monitor compliance, and inform patients about the side effects of medications.