Food For Thought: The Link Between Your Diet & Your Mental Health
With so much emphasis put on how the food we eat affects a persons physique and energy level, its important not to lose sight of how it can also affect ones state of mind.
Here, we explore the link between food and mental health, and how the digestive process directly influences your mood.
Having lived through a global pandemic, its safe to say its been a tough year and a half for most Canadians. Anxiety, loneliness and social isolation, uncertainty, fear of the virus, online learning, job loss and financial stress as a result of lockdowns have all wreaked havoc on our mental health. A poll conducted by Mental Health Research Canada in June 2021 indicated that 24 percent of Canadians reported selfrated high levels of anxiety, and 16 percent reported selfrated high levels of depression, compared with 8 percent and 7 percent, respectively, before the COVID19 outbreak.
The landmark 2017 SMILES Trial was a randomized controlled trial that looked at people with major depression. During the 12week study, participants were randomly placed into two groups, and received either social support or nutrition counselling to follow a Mediterraneanstyle diet. The Mediterranean diet is high in vegetables, fruits, whole grains, legumes , nuts, sources of healthy fats including olive oil, fish and seafood, includes small amounts of poultry, meat and cheese, and is low in sugar and processed foods like pop, baked goods, fast food, deli meats, processed snacks and the like.
In Conclusion Listen To Your Gut
Treat your second brain with care. Maintaining a healthy gut is the avenue to a more energetic, stress-free you. Pay attention to how your digestive tract is feeling and see if it lines up with whats going on in the mental health department. If youre feeling anxious and unmotivated, it might just be an issue with your microbiome. So embrace those beneficial bacteria and feed them well!
What Foods Help The Gut
A few groups of foods are specifically beneficial for the gut-brain axis.
Here are some of the most important ones:
- Omega-3 fats: These fats are found in oily fish and also in high quantities in the human brain. Studies in humans and animals show that omega-3s can increase good bacteria in the gut and reduce risk of brain disorders (
Read Also: Align Digestive Care Side Effects
Microbiota And Alzheimers Disease
According to the World Health Organization AD is the most common form of dementia and by far the greatest factor causing disability and dependency among older people around the world . The clinical picture of AD has severe physical, psychological, social and economic effects, not only on people with AD, but also on their caregivers, families and the society as a whole the socioeconomic consequences are dramatic and cannot be overstated. However, we still have no effective prevention and treatment strategy for AD .
Alzheimers disease is a degenerative disorder caused by polymerization of amyloid leading to the progressive loss of neurons. Interestingly, it has been recognized that amyloid can act as an antimicrobial peptide via activation of toll-like receptor 2 . However, it possesses harmful properties in a dysregulated state. Gut microbiota are a source of amyloid proteins sharing some structural similarities with amyloids from the CNS. The immune system could be primed by bacterial proteins in the gut enhancing immune response to endogenous productions of neuronal amyloid in the brain or they may act via molecular mimicry as prion proteins eliciting cross-seeding .
Pay Attention To Your Gut
The gut-brain connection is no joke it can link anxiety to stomach problems and vice versa. Have you ever had a “gut-wrenching” experience? Do certain situations make you “feel nauseous”? Have you ever felt “butterflies” in your stomach? We use these expressions for a reason. The gastrointestinal tract is sensitive to emotion. Anger, anxiety, sadness, elation all of these feelings can trigger symptoms in the gut.
The brain has a direct effect on the stomach and intestines. For example, the very thought of eating can release the stomach’s juices before food gets there. This connection goes both ways. A troubled intestine can send signals to the brain, just as a troubled brain can send signals to the gut. Therefore, a person’s stomach or intestinal distress can be the cause or the product of anxiety, stress, or depression. That’s because the brain and the gastrointestinal system are intimately connected.
This is especially true in cases where a person experiences gastrointestinal upset with no obvious physical cause. For such functional GI disorders, it is difficult to try to heal a distressed gut without considering the role of stress and emotion.
Recommended Reading: Can Tramadol Make You Constipated
How Gut Bacteria Can Affect Anxiety
It has long been understood that anxiety and depression are linked with our gut bacteria. Now scientists believe they have discovered tiny molecules in the brain that may be used by our gut bacteria to influence our emotions.
Our microbiome made up of 100 trillion bacteria has long been understood to have some influence over our mood and our mental health, but scientists have been unsure of exactly how.
Now a new study of mice suggests that gut microbes may alter microRNAs which are molecules that help keep cells in working order in the parts of the brain that control feelings of anxiety. The study which was published in Microbiome, could enable scientists to develop treatments for anxiety and other related mental health problems.
This research comes on the back of other exciting results into our gut microbiomes role in influencing our mental health. In one early study the presence or absence of certain gut bacteria was found to influence whether a mouse exhibits symptoms of anxiety, such as avoiding bright lights or open spaces.
What Was Remarkable Was That The Animals That Receive The Depressed Microbiome Behave Depressed
The researchers then dosed a group of germfree mice with lactobacillus bacteria the class of friendly bacteria that Phillips had also used on his melancholic patients. Although these mice still showed a higher stress response than the mice that had never been raised germ-free, their stress responses were less pronounced than the mice without any gut microbes.
There are even some signs that depressive behaviours can be transmitted across species from human to mouse through the microbes in the gut.
In one study, Chinese researchers in Chongqing took a sample of the gut microbiota from patients with Major Depressive Disorder and planted them in germfree mice. These mice subsequently were quicker to quit, on a “forced” swimming task a behaviour that is often considered to be analogous to the lethargy and hopelessness found in depression. And when the mice were placed in a box, they spent less time exploring the central areas and instead stayed closer to the edge, where they felt more secure.
What was remarkable was that the animals that receive the depressed microbiome, behave depressed, says Julio Licinio at New York Upstate Medical University, who was a co-author on the paper. If you change the microbiome, you change the behaviour.
Only two out of every 10 patients taking antidepressant drugs show signs of improvement
Multiple pathways
These effects may arise through many pathways.
Read Also: Does Peanut Butter Cause Heartburn
Gut Microbes Affect Inflammation
Your gut-brain axis is also connected through the immune system.
Gut and gut microbes play an important role in your immune system and inflammation by controlling what is passed into the body and what is excreted .
If your immune system is switched on for too long, it can lead to inflammation, which is associated with a number of brain disorders like depression and Alzheimers disease .
Lipopolysaccharide is an inflammatory toxin made by certain bacteria. It can cause inflammation if too much of it passes from the gut into the blood.
This can happen when the gut barrier becomes leaky, which allows bacteria and LPS to cross over into the blood.
Inflammation and high LPS in the blood have been associated with a number of brain disorders including severe depression, dementia and schizophrenia
Summary
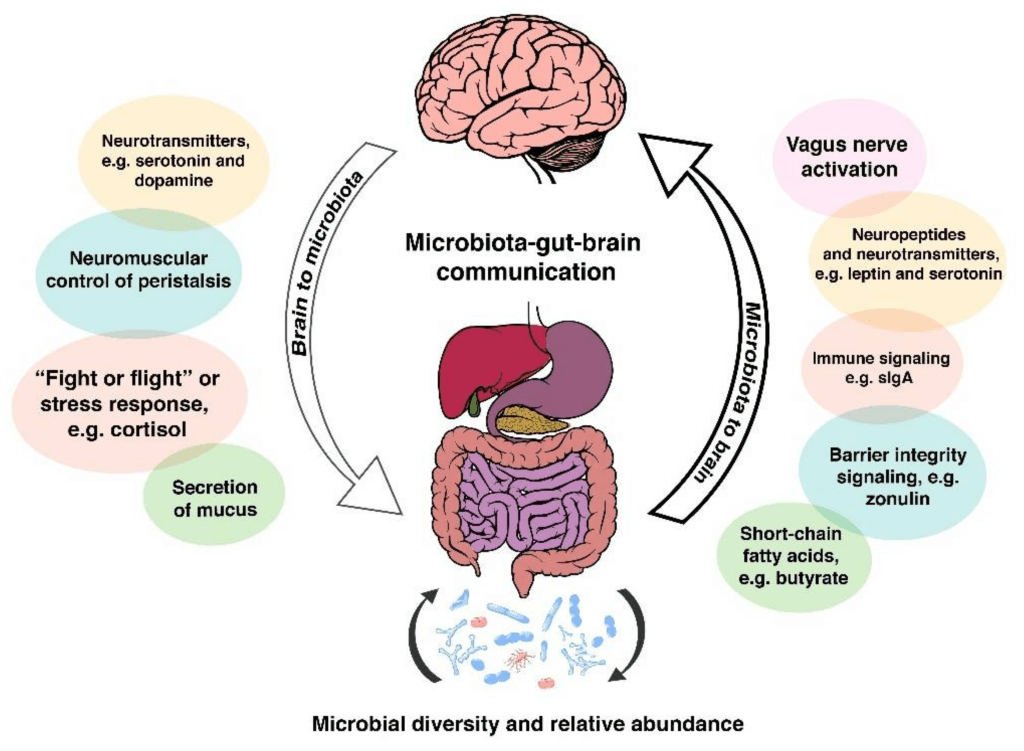
Your gut and brain are connected physically through millions of nerves, most importantly the vagus nerve. The gut and its microbes also control inflammation and make many different compounds that can affect brain health.
Gut Microbiota Imbalance Has Also Been Related To Some Neurological Diseases Such As Parkinsons Autism And Multiple Sclerosis Also In Nature Researchers From Harvard University Identified A New Gut
ALS is a fatal condition affecting motor neurons of the spine and the brain cortex. We know that apart from the genetic factors, there are also some environmental factors which can play a role. Again, this study showed that in mice with a common ALS genetic mutation, changing their gut microbiome could prevent or improve disease symptoms. The reason is that there are some bacteria that can stimulate the immune system and as ALS is an autoimmune disease in which the immune system overreacts, reducing the abundance of those bacteria you can improve the systemic inflammation or even autoimmunity and thus, mice mortality. However, these results from experiments on mice need to be confirmed in humans.
Also Check: Does Leaky Gut Cause Weight Gain
Weight Gain And Obesity
Gut dysbiosis has also been associated with weight gain and obesity through a range of mechanisms, including .
- Altered energy regulation
- Altered gut hormone regulation
- Promotion of inflammation due to pathogens entering the bloodstream via the intestinal wall .
Interestingly, overweight and obese people have been found to have lower gut microbial diversity compared with lean people .
One study compared 154 identical twins, one of whom was obese and the other whom was lean. The twins had significant differences in their gut microbiome composition, including the classes of microbes present and bacterial diversity. This suggests that differences in the microbiome are not genetic .
A similar study analyzed four pairs of twins. The gut microbiome from each twin was then introduced into mice. Despite the mice eating the same low-fat, high-fiber diet, the mouse hosting the obese twins microbiome gained more fat mass and presented more obesity-associated metabolic markers than the mouse hosting the non-obese twins microbiome .
Meanwhile, a long-term human study of 1,632 women found that low gut microbial diversity, especially in those with low dietary fiber intake, was associated with a higher degree of weight gain compared with those women who had a high microbiome diversity and fiber intake .
What You Eat Affects Them
Diet is one of the most important factors that shape the network of bacteria inside our colon. Weve seen how this happens. Here are some interesting facts to understand in what way diet affects your gut residents :
- Alterations in diet can even bring about changes in your microbiome in one single day!
- If these alterations are eliminated, your gut bacteria will return to normal within 48 hours.
- High-fat or high-sugar diets can affect these bacteria and alter your body clock too.
- In case of bodily stress, like a burn injury, the gut bacteria can take a hit within a day.
With these facts, it is understood that diet has a major impact on the composition of our gut microbiome. This fact has a great value for dietary strategies to manipulate the gut microbiome, especially during disease. Some prebiotic-containing foods are whole grains, beans, vegetables, fruits, garlic, bananas, onions, asparagus, and seaweed.
You May Like: Do Bananas Help With Bloating
The Gut Microbiome: Alterations Throughout Life
In healthy adults, the gut microbiota is dominated by only a few phyla, as noted above, and is characterized by a wide diversity of bacterial species. The human microbiome changes with age, normally becoming less diverse in the elderly as a result of higher numbers of Bacteroides species and reduced numbers of Clostridium groups. Even if the microbiome of adults is relatively stable when compared with that of infants or elderly, several factors can dramatically influence its composition over a relatively short period of time. Such factors include antibiotic treatment, stress, infection, host genetics, and diet.
Digestion And Other Roles: The Rent They Pay
Some bacteria get to work very soon after birth. One of the first occupants of our gut microbiome, Bifidobacteria, helps in digesting the healthy sugars in breast milk which are important for growth. Some bacteria help in digesting fibres.
This may help prevent weight gain, diabetes, heart disease, and the risk of cancer. The gut microbiome can also influence our immunity by communicating with the immune cells. About 70% of the immunity stays in the gut in the form of these microorganisms!
You May Like: How Much Bone Broth To Drink For Leaky Gut
Technical Approaches In Gut Microbiome Studies
Current technologies do not allow the cultivation of all bacteria isolated from the gut. Two widely adopted culture-free approaches have been devised to effectively quantify and characterize the microbiome, i.e., targeted sequencing and metagenomic sequencing. Targeted sequencing is also referred to as marker gene sequencing including 16S ribosomal RNA , internal transcribed spacer , and 18S rRNA sequencing. In 1977, Woese et al. inferred phylogenetic relationships between prokaryotic organisms using the rRNA small subunit genes this approach was later proven to also work well in eukaryotes . Wilson and Blitchington showed a good agreement of the diversity and 16S rRNA sequences between quantitative cultured cells and direct PCR-amplified bacteria from a human fecal specimen .
Researchers now can use this powerful tool to sequence 16S rRNA for assessing microbial taxonomy and diversity from various human specimens.
Other technologies including metatranscriptomics , metaproteomics , and metabolomics , can be applied to investigate RNAs, proteins, and metabolites in metagenome-wide association studies . The MWAS approach has shown great potential not only in the identification of the microbiome taxonomy but also in the annotation of functions, pathways, and metabolism.
Mechanistic Evidence Of Microbial Influence On Neuronal Signaling
Gaseous metabolites of bacteria, including carbon monoxide, hydrogen sulde, nitric oxide, and others, are also implicated in the neuronal control of gut functions by muscarinic cholinergic, vasoactive intestinal peptide., The interaction with the nerve cells is indirect and involves enteric glia, a collection of glial cells residing within the walls of the intestinal tract, and within epithelial and smooth muscle cells, interstitial cells of Cajal, and immune cells. Enteric glia are crucial for the above-mentioned interactions, as they also communicate with various types of non-neuronal cells in the gut wall, such as enterocytes, enteroendocrine cells, and immune cells and are therefore important local regulators of diverse gut functions. Several studies have emphasized the importance of enteric glia as modulators of ENS function, owing to the responsiveness of enteric glia to microbial, luminal, and inammatory signals.,, Thus, enteric glial cells regulate intestinal barrier function, immune responses, intestinal secretion, and gut motility and are hypothesized to be moderators of neurotransmission and neuroplasticity in the intestine.
Bile acids are also able to modulate neuronal activity, thus affecting both the host and microbiota, for example, by activating G proteincoupled bile acid receptors on intrinsic primary afferent neurons. This effect, however, depends on the specific bile acid, as some promote bacterial growth, whereas others inhibit it.,
Recommended Reading: Digestive Advantage Intensive Bowel Support Side Effects
Microbiota Altered Bloodbrain Barrier And Brain Structure
BBB is a semipermeable barrier composed of specialized endothelial cells in the microvasculature . The BBB separates the CNS from the peripheral blood . There are a variety of disorders related to microbial-induced BBB dysfunction, which may cause anxiety, depression, autism spectrum disorders , Parkinsons disease, Alzheimers disease, and even schizophrenia . The exact mechanism whereby the microbiota affects BBB physiology remains unknown. Possible mechanisms include BBB modulation by gut-derived neurotransmitters and bacterial metabolites. Rodent models have shown that a loss of the normal intestinal microbiota results in increased permeability of the BBB, while a pathogen-free gut microbiota restores BBB functionality . Metabolic diseases such as diabetes can result in increased permeability of the BBB and, potentially, further progression to Alzheimers disease with amyloid- peptide deposition . Microbiota dysbiosis has been found to alter the protective functions of the BBB, including regulation of permeability through tight junction expression or further behavioral changes .
How Does What We Eat Affect Our Brain
The composition, structure and optimal functioning of the brain are all dependent on the proper nutrients being available in the body. To start, the foods we eat actually become our brain cells. The brain is mostly made up of essential fatty acids, which we must get from our diet in the form of omega3 and omega6 fatty acids. Omega3 is found primarily in fatty fish, while omega6 is found primarily in vegetable oils. The typical North American dietwhich includes plenty of processed foods containing high levels of vege table oilshas more than enough omega6, but is often deficient in omega3, resulting in an unbalanced ratio of these two essential fatty acids. The problem is that omega6 has pro inflammatory properties, while omega3 has anti inflammatory properties. For this reason, getting enough omega3 and limiting highly processed foods is essential for the health of the brain.
Read Also: Can Align Probiotic Cause Nausea
How Gut Microbes Could Drive Brain Disorders
In 2006, soon after she launched her own laboratory, neuroscientist Jane Foster discovered something she felt sure would set her field abuzz. She and her team were working with two groups of mice: one with a healthy selection of microorganisms in their guts, and one that lacked a microbiome. They noticed that the mice without gut bacteria seemed less anxious than their healthy equivalents. When placed in a maze with some open paths and some walled-in ones, they preferred the exposed paths. The bacteria in the gut seemed to be influencing their brain and behaviour.
Foster, at McMaster University in Hamilton, Canada, wrote up the study and submitted it for publication. It was rejected. She rewrote it and sent it out again. Rejected. People didnt buy it. They thought it was an artefact, she says. Finally, after three years and seven submissions, she got an acceptance letter.
John Cryan, a neuroscientist at University College Cork in Ireland, joined the field about the same time as Foster did, and knows exactly how she felt. When he began talking about the connections between bacteria living in the gut and the brain, I felt very evangelical, he says. He recalls one Alzheimers disease conference at which he presented in 2014. Ive never given a talk in a room where there was less interest.
Credit: Nik Spencer/Nature