Should Children Take Probiotics While On Antibiotics
Another well-known approach to prevent or relieve diarrhea from antibiotics is taking a probiotic. Research suggests there may be some preventive benefits to taking probiotics when starting an antibiotic. However, Dr. Gurram cautions not to take all the research at face value. For instance:
- There are inconsistencies in the research about the number of probiotic bacteria needed to restore gut flora and which probiotic is best.
- Probiotics are considered nutritional supplements and not regulated by the FDA. There is no guarantee the product will have the dose or amount it claims to include.
- Many of the manufacturers of probiotics sponsor the research, which could lead to a conflict of interest.
“A probiotic may help prevent one episode of antibiotic-associated diarrhea in about 12 to 40 children who take it,” Dr. Gurram explains. “It’s just really difficult for a probiotic to restore the body’s microbiome because there are so many different strains of bacteria in the gut.”
The Bottom Line On Antibiotics And Gut Health
Antibiotics, as helpful as they are to quell a bacterial assault , interact with our cells, particularly immune cells, in ways that we really dont understand. The biochemical changes matter when the outcome is uncertain and the possibility of spawning antibiotic resistance is real. To help resurrect cells that have been denigrated by their rescuer, pre- and probiotics have the means.
Antibiotics Effect On Gut Health
Until a few decades ago, many healthcare researchers were of the view that a sterile body is the healthiest one.
However, the medical community now recognizes the effects and benefits of microorganisms, including bacteria for the human body but no one says Ruffles potato chips and 7UP is healthy to consume throughout the week but that did not deter Louie Lastik from Remember The Titans who obviously did not know how to eat right though this is another topic.
Researchers say that there is a whole world of good and bad microorganisms residing in your intestines, and keeping them in balance keeps you healthy. However, a course of antibiotics can seriously disrupt this balance and have powerful effects on the composition of the gut microbiome.
Here is everything you need to know about antibiotics, how they affect your gut health, and ways to recover afterwards.
Recommended Reading: Probiotics Inflammatory Bowel Disease
How Does Antibiotic Resistance Develop
Bacteria can evolve into superbugs in a couple of ways. The first way is through genetic mutations that cause them to become resistant to certain antibiotics. Another and the most effective way in which superbugs evolve is through gene transfer. Bacteria are capable of engaging in gene transfer, whereby they can pass along genetic information to one another.
Gene exchange among bacteria has increased the speed at which bacteria has been able to evolve mechanisms to become antibiotic resistant. One such mechanisms is known as a biological pump, in which enzymes degrade antibiotics and wash them out before they take effect.
An Overview Of Gut Microbiota
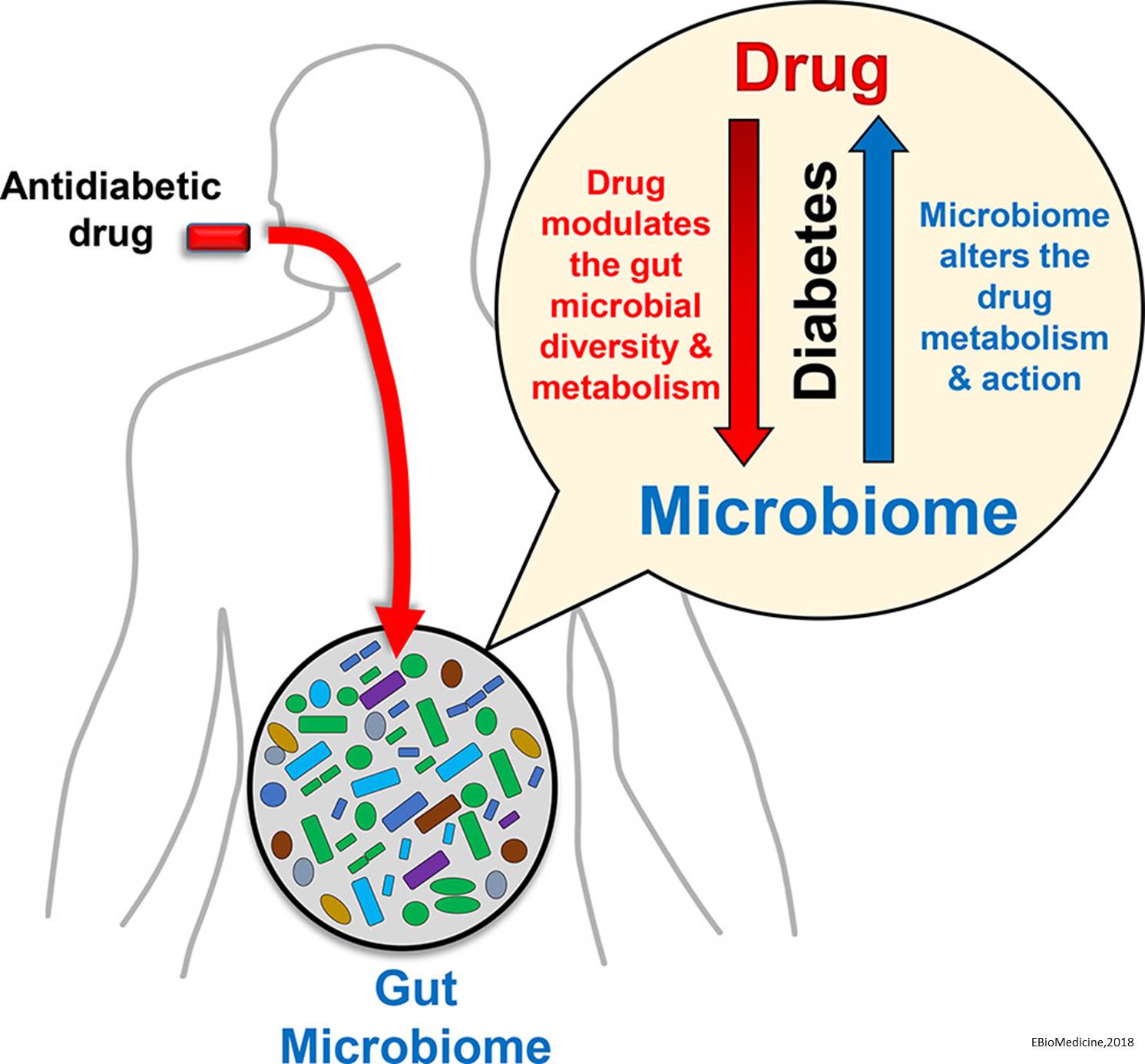
The gut is the largest reservoir for microbiota in mammals and humans. However, our understanding of gut microbes has been limited for a long time because most gut microbes cannot be identified by traditional culture technology. Recently, the rapid development of high-throughput sequencing technology, including metagenomics, metatranscriptomics, and metaproteomics approaches, has provided us with powerful tools to study the composition and function of gut microbiota. It is estimated that approximately 100 trillion microbes from over 1000 species and more than 7000 strains reside in the gut. Although enormous gut microbes in addition to bacteria have recently been identified , bacteria are still the main participants in gut and host homeostasis.
The five major bacterial phyla in the gut are Firmicutes, Bacteroidetes, Actinobacteria, Proteobacteria, and Verrucomicrobia, accounting for more than 90% of the total bacterial population that inhabit the gut. The rest of bacteria are from less abundant phyla, such as Fusobacteria and Fibrobacteres. These microbial communities reside with varied density in different segments of the gut and play a crucial role in many aspects of physiological processes, including facilitating food digestion and energy utilization, synthesizing vitamins and essential amino acids, promoting the development of the immune system, maintaining the integrity of the gut mucosal barrier, and protecting against enterogenous pathogens.
Also Check: Does Tramadol Cause Heartburn
Can Some Peoples Gut Bacteria Recover From Antibiotics In Around Six Months
Some research released in 2018 found that it took around six months for our gut flora to get back to normal after antibiotics . The media picked up on it, and so a lot of people today think that you get your old gut back precisely six months after antibiotics. This study is just one of many though, all with different results.
If youre feeling overwhelmed by all this information, you can get some strategic help with our no obligation symptom checker.
Its possible that your gut bacteria might never return to normal. But that doesnt mean that you cant take steps to increase your diversity. Everyone can benefit from taking care of their gut, but if youve taken antibiotics recently theres an even bigger reason to do it.
Consider Natural Alternatives To Antibiotics When Possible
Livestock and poultry live in such proximity to each other that they share more than food. They stand in it, they wallow in it, and they breathe it. How does the farmer in the dell protect his animals from catching each others sicknesses and diseases? From cattle to chickens, and probably even to farmed fish, antibiotics have been necessary evils, having resulted in tremendous increases in animal production and protection of human health. Its been a rare case when these drugs werent used. Some factory farms that swore they were antibiotic free were later found to be in violation of the truth. Primary care physicians prescribe antibiotics to satisfy their patients false beliefs that this class of drug will cure their common cold and remove symptoms of influenza. Whats wrong with this? Antibiotic resistance is the concern, an issue that develops almost too quickly for science to keep ahead of the pathogens.
Enter the alternativesthe natural antibiotics.
Read Also: Can Align Probiotic Cause Nausea
Medications That Can Harm Your Microbiome And What You Can Do
Each day it seems were learning more about the marvelous miracle that is our intestinal microbiome the collection of bacteria, yeasts, and viruses that live in our gut and do an enormous amount of work to keep us healthy. Amongst the many accomplishments our microbiome could boast are manufacturing vitamins , detoxifying environmental toxins , keeping our mind and mood steady, and keeping our weight down and regulating inflammation. We also know that what we put in our bodies, from foods to medications, has an impact on this precious reservoir of organisms.
The impact of antibiotics, and particularly the rampant antibiotic overuse that has become so prevalent, on our gut microbiome has become increasingly evident as research continues to emerge on the importance of our microbiome to our health. Disruptions in the microbiome have been associated with diabetes, weight problems, anxiety, depression, autoimmune disease, sugar cravings, fatigue, PCOS, fertility, immune health, adrenal dysregulation, and much more.
Did you know that:
Yet most of the antibiotics being prescribed doctors are unnecessary and harmful to us personally and globally. Learn what you can do to protect yourself from antibiotic overuse, and help reverse a very alarming and dangerous public health problem.
Antibiotics Have Their Place
Antibiotics are one of the most important medical innovations and save lives when used appropriately. But inappropriate use leads to potentially untreatable resistant infections and long-term health problems in children and adults.
A recent assessment predicted that without restrictions, global antibiotic use will increase three-fold by 2030. Unless we all work together to reduce antibiotic overuse, we could be assigning our children to a future of chronic ill health. Too much too young underappreciated long-term adverse effects of early antibiotic exposure
Recommended Reading: Does Famotidine Make You Sleepy
Alterations Of The Gut Microbiome By Antibiotics
Antibiotics, as lifesaving medicines for over a century, have been in the front line for combating infections, preventing various medical conditions, and promoting animal growth . However, they present certain disadvantages including antimicrobial resistance and adverse drug events . As gut microbiota is characterized by multiple shifts from the endometrial period till the end of life, antibiotics are suggested to represent one of the most pivotal factors for these alterations stimulating or promoting various diseases.
Since 1940, it has been known that antimicrobials may affect the intestinal microbiota. In 1950, terramycin proved to alter the gut microbiota in patients submitted to bowel surgery . Dysbiosis is closely related to the use of medication, being characterized by the flourishing of the pathobionts, i.e., resident microbes with pathogenic potential the loss of -diversity, i.e., the mean species diversity in the intestinal tract the recruitment of inflammatory cells the leaky gut syndrome and the impaired protection against pathogens . Figure 2 depicts the main mechanisms interconnecting gut dysbiosis triggered by environmental exposures such as diet and antibiotics and obesity.
Fig. 2
Antibiotics And The Animal Microbiome
The weaning practices that take place in farms influence the animals microbiome and create a false need for antibiotics. As Evans explained in her talk, piglets are taken away from their mothers too early that is, before theyve had a chance to develop a strong immune system or a healthy, fully matured gastrointestinal tract.
For example, piglets would naturally wean when they are around 34 months of age.
In the U.S., however, piglets are weaned when they are 1728 days old.
Evans explained that not having access to the natural antibodies present in the mothers milk impacts the animals immune system. Abrupt weaning has also been found to raise the risk of gastrointestinal disease in calves and lambs.
In turn, these diseases call for the use of antibiotics, sometimes prophylactically. For instance, piglets, calves, and lambs can have post-weaning diarrhea and associated infections, so farmers give them antibiotics to prevent such infections.
Also, Evans explained in her talk, a pigs microbiome is colonized at birth and subsequently modified during the suckling period and the weaning period. During this time, the gut microbiome diversifies.
However, between beneficial and harmful bacteria in the gut.
Furthermore, genomic studies cited by Evans have found a dramatic increase in Escherichia coli in the pigs small intestines after receiving antibiotics. E. coli is responsible for half of all piglet deaths worldwide.
Read Also: Can Align Probiotic Cause Nausea
Microbiome And Host Immune Maturation Are Intertwined And May Affect Vaccine Efficacy
Perinatal microbial exposures, proper timing of these exposures, subsequent assembly of the microbiota, and early-life milestones in mucosal and systemic immune system maturation are all intertwined . These interdependencies have relevance for early childhood responses to vaccines. Microbial priming of the immune system probably begins before birth. Experiments in mice suggest that maternal gut colonization patterns during pregnancy affect intestinal innate lymphoid cells in the newborn, which in turn prevent intestinal inflammation in the pups . Transient colonization of the dams during gestation led to improved intestinal barrier integrity and systemic immune responsiveness. It was proposed that these effects were mediated by maternal microbiota products transferred to the offspring by antibodies.
As we look forward, new strategies for addressing AMR should exploit these connections between microbiome and immune system. One might consider targeted manipulations of the microbiome that induce or reinforce protective host responses against clades of resistant organisms and enhance protective responses to vaccination, thereby minimizing the need for antibiotics. For example, the deliberate selection, design, and testing of probiotic sets of strains for use in early childhood to stimulate protective and nonallergic immune responses deserves a great deal more attention.
The Misuses And Abuses Of Antibiotics
The problem with antibiotics is not entirely the antibiotics themselves. They are life saving drugs and many of us owe our lives to their discovery, but the over consumption of them is leading to their ineffectiveness. Some of the ways antibiotics are misused are easily avoidable. Below we outline two of the most common ways antibiotics are abused.
Recommended Reading: Align Digestive Care Side Effects
The Length And Number Of Courses
Multiple courses of antibiotics appear to be the most damaging , and higher doses of antibiotics taken over a longer period of time have the biggest impact. This might be shocking news to the many people whooften as teenagerstook antibiotics for months on end in an attempt to treat their acne.
Oluf Pedersen, chief scientist on a 2018 project that looked at the impact of just one course of antibiotics on the microbiome, pointed out that most people will get multiple rounds of exposure to antibiotics. The concern relates to the potentially permanent loss of beneficial bacteria after multiple exposures to antibiotics during our lifetime, he said to journalists for the science news website ars TECHNICA.
Does The Gut Microbiome Ever Fully Recover From Antibiotics
Most gut bacteria recover quickly, but there can be long-lasting consequences from taking antibiotics.
Q. What are the consequences of taking antibiotics on your gut microbiome? Does the gut ever fully recover?
A. Most gut bacteria recover quickly, but there can be long-lasting consequences from taking antibiotics. The changes, however, are not necessarily harmful.
The gut microbiome, the roughly 10 trillion to 100 trillion bacteria and other microorganisms that live in the digestive tract, contributes to health by synthesizing vitamins, metabolizing drugs and fighting pathogens. Anything that disrupts the balance of microorganisms, such as antibiotics, which can kill both good and bad bacteria, has the potential to cause disease.
Data from a 2016 study suggest that exposure to antibiotics in infancy can alter the gut microbiome and weaken the immune response for years to come. Other studies have linked the use of antibiotics in children to an increased lifetime risk of asthma, obesity and inflammatory bowel disease, effects thought to be mediated by the gut microbiome.
In an example of a potentially beneficial effect of altering the gut microbiome, evidence suggests that antibiotics can suppress the formation of a molecule in the gut that increases the risk for heart disease.
Do you have a health question?Ask Well
Don’t Miss: Why Is My Ibs Worse In The Morning
Avoid Sugar And Processed Foods To Control Growth Of Candida
Some people taking antibiotics can develop candida or yeast overgrowth, such as in the vagina or mouth. Broad-spectrum antibiotics can wipe out microorganisms that keep the environment acidic, preventing the growth of yeast. One of the ways how to heal gut flora after antibiotics are to avoid sugar since yeast tends to feed on them. Yeast thrives on sugar, so reducing your sugar intake will directly reduce your risk of a yeast infection. Without cutting back on sugar, yeast can take over and cause some health problems.
Although, while you are reducing your intake of sugar, you should also not consume too many artificial sweeteners. Artificial sweeteners are popular replacements for sugar. However, there have been studies shown that artificial sweeteners can harm your gut microbiota.
Development And Maturation Of The Microbiome
As a child grows, the commensal microbiota develops in a predictable succession of species that is generalizable across human populations . The developing bacteriome, the bacterial component of the microbiome, has been profiled many times, both taxonomically and in terms of metabolic functions . These profiles have provided a view of how bacterial species are structured over time. Less is known about the gut-associated eukaryotes and viruses that develop along with the bacteriome, although they are an important part of the gut ecosystem . The disruption of the bacterial succession can be pathogenic . Critical developmental milestones for the microbiota occur, in particular, during infancy and early childhood, and both medical intervention and lack of such intervention during these periods can have lifelong consequences in the composition and function of the gut ecosystem . In this section, we discuss the instances in which antibiotics are often used during development and adulthood, the effects of antibiotics on the microbiota, and the implications of such effects for health and disease.
Fig. 1
Health consequences linked to the disruption of human-associated microbiota involving antibiotic use during development and adulthood. Red lines indicate that a single dose of antibiotics within the time period has been linked to a health consequence, whereas a dotted red line indicates that multiple doses of antibiotics within the time period are required to observe a link
Read Also: Does Pickle Juice Help Heartburn
Skip Gluten And Dairy To Reduce Food Sensitivities
Taking antibiotics is like carpet-bombing your gut flora: they can lead to mass die-offs of microorganisms, including the good ones. Since the diversity of your gut flora plays a significant role in metabolism and immunity, you may develop food sensitivities after your medication plan. One study suggested antibiotics can influence the risk of childhood food allergies. After completing your medications, you may want to avoid the common culprits of food intolerances such as dairy and gluten, which is a protein present in wheat.
For this reason, you may find it beneficial to eat a plant-based diet after taking a course of antibiotics. Especially to heal gut flora after antibiotics to treat an infection. Studies have shown that vegetarian diets can benefit your healthy gut microbiota. This happens because of the high fiber content in many vegetarian foods. By following a vegetarian diet, you can reduce the levels of bacteria that cause diseases, as well as losing weight, reducing inflammation, and cholesterol levels.
While diets that contain animal-based foods promote the growth of different types of bacteria than plant-based diets do. Vegetarian and vegan diets can improve healthy gut microbiota. Although, it is unclear whether the positive effects are a result of a lack of meat.