Two Doctors Talk About What Ovarian Cancer Pelvic Pain And That From Irritable Bowel Syndrome Are Like
Pelvic pain can be caused by ovarian cancer. It can also be caused by IBS. Do they feel alike? What are the differences?
Lets first start with the pelvic pain from ovarian cancer. For this topic is Teresa P. Diaz-Montes, MD, of the Gynecologic Oncology Center at Mercy Medical Center, Baltimore, MD.
Dr. Diaz-Montes first notes that the pelvic pain is usually local to the pelvis: the lower abdominal area, beneath the belly button.
The pain could be more localized to one side of the pelvis depending on the size and location of the ovarian mass, she says.
The pain is usually constant and not aggravated by movement. It can be associated with a sensation of pressure in the pelvis.
A women may complain of a new onset of constipation or urinary frequency .
This is due to the compression of the pelvic mass on the adjacent organs.
If the mass is too big, it may be able to be palpated on examination. This can also cause abdominal distention and the sensation of bloating.
The intensity of the pain depends of the size of the mass. When the ovarian mass is small, the pain is dull and described as a discomfort.
When the mass is larger, the pain could be very intense and sharp, requiring the use of pain medications.
For pelvic pain associated with irritable bowel syndrome, the physician is Nnenna C. Okpara, MD, gastroenterologist and director of endoscopy at the Center for Womens Gastrointestinal Health, Women & Infants Hospital in Providence, RI.
Common Ibs Symptoms In Females
Irritable bowel syndrome is an intestinal disorder that affects up to 11% of the global population. Among IBS sufferers, only about 30% seek treatment from a physician for their IBS, particularly if those symptoms present alongside other conditions.
Which gender is more likely to have IBS? Women are more likely to have IBS than men, especially if they also have a family history of IBS. According to a 2018 study, Sex hormones and gender differences may play important roles in the pathophysiology of IBS.
Some women experience worse IBS symptoms during their menstrual cycles, making this condition even more difficult to diagnose.
What is the most common symptom in a woman with IBS? The most common symptom in a woman with IBS is abdominal pain, often associated with constipation. This may be caused by colon spasms or other causal factors.
While many symptoms overlap with symptoms found in male IBS sufferers, some are unique to women. There are 13 common IBS symptoms in females to look out for to assist in diagnosis and plan for treatment, including:
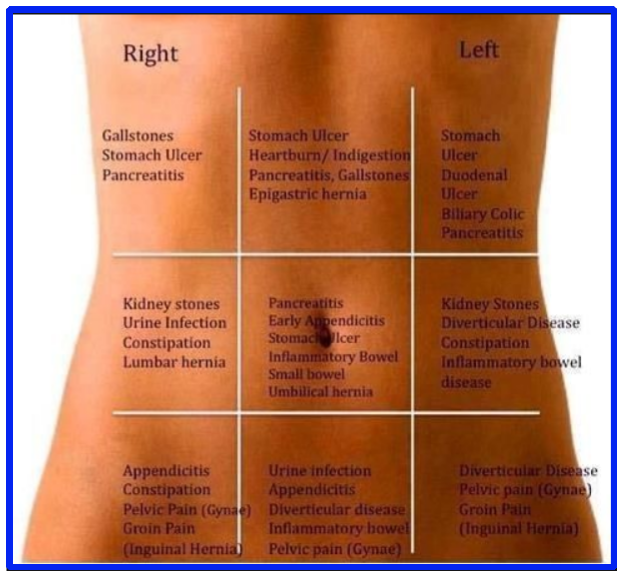
Ibs Pain Around The Umbilicus :
IBS pain is commonest in the lower abdomen, especially around the umbilicus. IBS Pain located around the umbilicus retains the typical IBS characters:
- Colicky in nature: with waves of colon contractions followed by waves of partial relief.
- Associated with gas distension and bloating.
- Usually increases after meals.
- Related to defecation: may become relieved or increased during or after you poop.
- Recurrent, but not progressive: this means that you experience IBS at least once per week for at least the previous 3 months. Usually, there are periods of remissions and flare-ups .
But if the pain becomes progressive you should consult your doctor.
Other conditions causing pain around the umbilicus :
- Early appendicitis.
You May Like: Does Baking Soda Help Heartburn
Treatment Approaches For Ibs
When pain is chronic it takes time for it to go away. Because pain is an emotional experience, taking steps to improve emotions can lead to reduction of the harmful effects of the pain even when it is still present.
Maintaining an active role in life, engaging in physical activity, and addressing emotional and social health are important to help promote a sense of well-being, which counters negative expectations.
- Medications
- Anticholinergic agents taken before a meal can provide short-term relief. These gut-targeted medications work on several IBS symptoms, including pain, diarrhea, and constipation.
- Central acting agents, or central neuromodulators, can block signals from the brain. This type of drug can help decrease intestinal and central hypersensitivity, help the brain control the pain, and improve gut motility. Central acting agents use two approaches to help reduce pain. In the first approach, the medication helps the brain to limit nerve signals by closing the gate to pain. In four to six weeks, the pain is generally 30%50% better. The second approach involves helping to regrow the damaged nerves. Regrowth takes a long time anywhere from six months to a year or more. Creating new functioning nerves is vital to prevent the pain from returning.
- There is no evidence that opioids can help IBS. In fact, taking opioids can slow the gut, causing constipation, nausea, and vomiting. Learn more about opioid-Induced constipation
What Can Be Done To Help
We see many commercials on television today about medications that can help ease the symptoms of IBS. These medications can help ease cramping, diarrhea, constipation, and bloating. Although these treatments are helpful, a combination of diet changes, such as removing gluten, going on the FODMAP diet, removing carbonation and alcohol from your diet, and exercise can all will help to improve symptoms and quality of life for those suffering from IBS.
IBS and chronic pelvic pain are multifactorial conditions for which there is not a one size fits all treatment. Our pelvic floor specialized therapists will partner with you to create a customized treatment plan. The treatment plan may include trigger point dry needling to the pelvis, hips, and back, pelvic floor exercise, biofeedback training, manual therapy to the pelvic floor, back, hips, and internal organs, education, and exercise program development.
Dont wait any longer in seeking treatment for symptoms and pain associated with IBS and chronic pelvic pain. Schedule your appointment today with one of our highly trained pelvic floor specialists.
Also Check: Align Women’s Health Prebiotic And Probiotic
Higher Risk Of Endometriosis
Research has shown that women who have IBS have a higher risk of being diagnosed with endometriosis.
If you have this gynecological disorder, tissue that forms the lining of your uterus will grow outside of your uterine cavity. This is called endometrial tissue, and it can then grow on your ovaries, bowels, and tissues lining your pelvis.
Endometriosis is painful and can cause extreme discomfort, serious PMS symptoms, and even infertility.
Overlap Between Cpp And Ibs
The expected overlap of IBS and CPP was calculated by multiplying the corresponding marginal proportions , and compared with the observed overlap . The observed numbers for overlap of IBS and CPP were about 2 times higher than the expected numbers . The overlap of IBS and CPP was significantly higher than expected by chance alone .
Risk factors for reporting overlap of IBS and CPP versus pure IBS or CPP are shown in Table 2. A high somatic symptom checklist score, depression, dizziness, and weakness were associated with a significantly greater odds for reporting overlap of IBS and pelvic pain compared to the pure IBS group. A high somatic symptom checklist score, headache, depression, and dizziness were associated with a significantly greater odds for reporting overlap of IBS and pelvic pain compared to the pure CPP group. The overlap group of IBS and CPP was not significantly associated with greater physician visits, physician visits for aches or pain, physician visits for bowel problems, or hospitalizations compared to the pure IBS or CPP alone group.
You May Like: Can Omeprazole Cause Ibs
Suffering From Ibs You Also Should Get Checked For Endometriosis
About 15 percent of adults in the U.S. suffer from irritable bowel syndrome , the majority of whom are women.
Women account for nearly 65 percent of all cases of IBS, a condition that affects the large intestine and leads to painful symptoms such as cramping, abdominal pain, constipation, diarrhea and bloating.
IBS causes a lot of discomfort for many women, and its symptoms often resemble another serious womens health issueendometriosis.
Endometriosis is a gynecological disorder in which the tissue that normally lines the inside of the uterus begins to grow outside of it, leading to severe abdominal and pelvic pain. Endometriosis sometimes involves the ovaries and can affect your reproductive health.
Aside from painful periods, some of the most common symptoms of endometriosis are constipation and painful bowel movements, especially during your period.
The Link Between IBS and Endometriosis
According to the UNC Center for Functional GI and Motility Disorders, women with IBS are more likely than women with other bowel symptoms to be diagnosed with endometriosis. But conversely, some women who experience bowel issues may be misdiagnosed with IBS when in fact they have endometriosis.
When to See a Doctor
So, how can you tell the difference between IBS and endometriosis? And when should you be concerned that bowel issues may actually be endometriosis? Unfortunately, the answer isnt that simple.
Pelvic Pain And Irritable Bowel Syndrome
According to a 2006 study in the American Journal of Obstetrics and Gynecology, irritable bowel syndrome often goes unrecognized and untreated in women with chronic pelvic pain. Pain in the pelvic region may be steady or intermittent, and is considered chronic if it lasts for six months or more. It affects between 33-39% of women at some point in their lives. The relentless pain which may be caused by any organ system or disease and may have multiple contributing factors reduces quality of life for sufferers.
IBS is a chronic, often debilitating, functional gastrointestinal disease with symptoms of abdominal pain, bloating, and altered bowel habits such as constipation or diarrhea, or both. IBS is estimated to affect 13-20% of Canadians, and is significantly more common in women than in men.
In a study spanning the years 1993-2000, researchers from the University of North Carolina at Chapel Hill surveyed 987 female patients at a chronic pelvic pain clinic. Thirty-five percent of the women met the Rome I criteria for IBS but almost half of these women had not received a diagnosis of IBS from their physicians. Additionally, more than 67% of the women who were diagnosed with IBS did not receive any treatment recommendations from their physicians. The researchers suggest that the diagnosis and treatment rate is even lower in a general gynecology office than in this specialized chronic pelvic pain clinic.
Image: siam.pukkato | bigstockphoto.com
Email News Sign Up
You May Like: Diarrhea Medicine For Pregnancy
Accompanied Symptoms With Testicular Pain
Several other signs and symptoms can accompany IBS testicular pain. You must be alert and look out for your symptoms to prevent the condition from getting worse. Make sure to consult your general physician. Tell them your observations precisely.
The other signs and symptoms with testicular pain may include:
- Your testicles may feel tender upon touch
- Redness or erythema of the testicles may be observed
- Swelling may be present, and they may become larger in dimension
- The pain may be accompanied by fever
- You might feel pain while urinating
- Excessive pain may lead to nausea and vomiting
- Penile discharge may be present
- You might have painful sexual intercourse
- Pain during ejaculation may be present
- Blood may appear in the urine
- Specks of blood may be present in ejaculation
Testicular pain on its own is an annoying condition. However, you should keep an eye out for other symptoms as well.
Risk Factors For Ibs In Women
Women face a number of additional risk factors for IBS, such as:
- Age: IBS symptoms in women typically present before 50, during a womans menstruation years. It is very rare for a woman to report her first IBS flare-up after 50.
- Family history: Women with a family history of IBS are at higher risk for developing the condition. Researchers suggest environmental factors play an essential part even in these cases where genetics may be involved.
- A history of abuse: IBS and other functional disorders are reported at a much higher rate in women with a history of sexual abuse. This may be linked to IBS triggers associated with abuse, such as sleep disruption and mental health disorders.
- Fibromyalgia: IBS often coexists with functional disorders like fibromyalgia. Mental health conditions associated with chronic pain also worsen IBS symptoms. Some providers suggest antidepressants, but its important to get to the root of your symptoms, as well.
- Intestinal infections: Some patients experience their first IBS flare-up following a bout of stomach illness or infection. That can include gastroenteritis, or stomach flu. This is referred to as post-infectious IBS.
You May Like: Can Stress Cause Gerd To Flare Up
When To See A Doctor
Testicular pain should be treated as an emergency until proven otherwise. If you feel discomfort or pain, contact your doctor immediately. There might be instances where the pain is too much to handle. Go straight to the emergency room if something like this occurs.
Urologists, oncologists, and general surgeons specialize in such conditions. Your general physician should be able to treat basic problems. But, If there are underlying conditions, then a specialist might need to get involved.
Your doctor may perform a physical exam. They may also run blood tests, urethral swab cultures for checking STDs and discharge. They might take urine tests. Ultrasonography and nuclear exams might also help to identify the condition.
If you are experiencing testicular pain, then you shouldnt wait. Sometimes digestive problems and testicular pain can be connected too. Thus, you should take steps and contact your doctor as soon as possible.
Food Poisoning & Joint Pain
Food-borne illnesses are also highly associated with both gastrointestinal symptoms but also joint pain.
Post-infectious symptoms may not manifest for weeks or months following exposure, but a clear link has been linked with reactive arthritis.
This is believed to take place due to the potentially harmful organisms reaching the general circulation, which activates specific immune cells called T-cells.
It is then possible for these T-cells to mistakenly attack the tissue in the joint by mistake leading to an inflammatory response and pain.
Read Also: Does Tramadol Cause Bloating
How To Relieve Testicular Pain
There arent many easy home remedies for IBS testicular pain. You shouldnt endure it instead, you should visit your general physician as soon as possible. The doctor needs to identify your condition correctly. Only then itll be easier to prescribe drugs to relieve the pain.
You can take some over-the-counter painkillers to get temporary pain relief. The pain killers may include acetaminophen, paracetamols, Tylenol, etc. Be careful not to give children aspirin as it increases the risk of Reyes disease.
The doctor might prescribe you the following treatments
- Antibiotics in case an infection has occurred
- Painkillers for pain relief
- Use of ice to provide comfort
- Use of scrotal support to avoid discomfort
- Surgery
Signs And Symptoms Of Testicular Pain
You might feel IBD and testicle pain for several reasons. The criteria of pain vary from person to person. Some people complain of dull and numbing pain. Some patients complain about pain before and after releasing bowels.
The pain may come in waves. It sometimes feels like a sharp, stabbing pain. The pain may persist for several days, then go away on its own. It comes back after a few days. Patients have also complained about shrinkage of testicles and persistent pain.
The pain may be aggravated while changing positions. Usually, it is a dull ache, and you may feel tenderness while palpating your genitals. The pain may spread as right testicle pain and lower abdomen pain to your abdomen and posterior side.
Recommended Reading: Salad Causes Gas
You Might Also Like One Of These:
- How to relieve trapped gas Need some help letting it go? These practical tips will help you prevent trapped gas when you can and relieve it when it strikes.
- Why do your IBS symptoms flare on your period? Have you ever noticed your IBS symptoms always seem to flare up during your period? Here’s everything you need to know about how and why your cycle can throw a monkey-wrench in your gut!
- Is your abdominal pain related to IBS?Have you ever felt a sharp pain or cramp in your abdomen and wondered if it was caused by your IBS? Here’s what you need to know about IBS and abdominal pain!
If you like this post, don’t forget to share it! Together we’ll get the low FODMAP diet down to a science!
What Treatment Is Available For Irritable Bowel Syndrome
Your health care provider will create a care plan for you based on:
- your age and your health history
- the seriousness of your case
- how well you handle certain medicines or treatments
- the course of action you prefer
Treatment for IBS may include:
Dietary changes. In some cases, a high-fiber diet can reduce symptoms. Some people whose symptoms are triggered by lactose should eat lactose-free dairy products, while others are affected by poorly digestible carbohydrates and fructose. Some people are intolerant to gluten, though they may not have celiac disease. Many people have symptoms after large and fatty meals. Keep a list of foods that cause you pain, and discuss it with your physician.
Medicines. Your health care provider may prescribe fiber supplements or have you take a laxative now and then to soften your stool. Different medicines are used for IBS, depending on your symptoms. These prevent constipation, diarrhea, pain, and spasm.
Antibiotics. An antibiotic is used in certain situations to improve irritable bowel syndrome symptoms, especially bloating, distention, and loose stool.
Natural supplements. Some people feel better on various natural supplements called probiotics. Others get relief with peppermint oil capsules.
Manage stress. Hypnosis, acupuncture, cognitive therapy, yoga, regular exercise, relaxation, and other mindfulness activities can help some people.
Also Check: Who Sells Align Probiotic