The Basics Of Autoimmune Diseases
Autoimmune diseases refer to any conditions that cause the immune system to attack the body. The immune system is important because it wards off infections and helps fight viruses. Common autoimmune conditions include Type I diabetes and lupus. With diabetes, the body stops regulating and processing the sugars that the person eats. Many patients need to take daily doses of insulin to treat the condition. Other conditions can cause the body to view any abnormality as a threat and attack healthy cells and organs.
Fatigue is a common symptom of autoimmune conditions. Some people feel tired because their bodies do not produce enough hormones, but others feel tired because they keep waking up at night due to their conditions. People should talk with their primary care physician about any unusual symptoms they experience, especially if they have a family history of these autoimmune diseases.
Couple Conflicts Raise Risk For Leaky Gut
Here’s another way to protect against leaky gut: don’t bicker with your spouse or partner, suggests a study in the December 2018 Psychoneuroendocrinology. Researchers had 43 healthy married couples discuss and resolve a conflict likely to provoke a strong disagreement, like a money problem. Blood samples taken afterward showed high levels of LPS-binding protein, a biomarker for leaky gut, among couples that argued more compared with couples who were calmer.
Healing Your Gut Is The 1st Step To Reversing Autoimmune Disease
Autoimmune diseases are diseases of the immune system. As around 80% of your immune cells are located in the gastrointestinal tract, gut health is closely linked to immune function.
Research shows that the digestive condition known as leaky gut , is a common factor in the biological mechanism that leads to the onset of autoimmune disease.
While it is easy to make the connection between the gut and digestive conditions such as food allergies, Celiac disease, Crohns Disease, and Ulcerative Colitis, the link to autoimmune disorders such as Type 1 Diabetes, Multiple Sclerosis or Rheumatoid Arthritis etc can be a little harder to grasp.
So, lets break it down.
Firstly what exactly is the Gut?
The word gut is another way of referring to your gastrointestinal tract or digestive system. Put simply, the gut is the passage through which food enters your body through your mouth, is digested in your stomach, beneficial nutrients are absorbed in your intestines and then toxins and wastes are expelled via the rectum.
The innermost surface of the gut is known as the intestinal barrier.
This barrier is semipermeable as it allows certain substances to pass through it but not others. It is the role of this barrier to protect the body by only allowing nutrients, water and electrolytes to cross into the blood stream while preventing undesirable substances from entering the body by retaining them in the gut to be excreted as waste.
How does the gut become leaky?
Vicky Ellenport
You May Like: Can Peppermint Tea Help With Constipation
Use Nutrients And Herbs To Help Intestinal Cells Recover
In addition, consciously and intentionally including some key nutrients as well as gut-healing herbs in your diet every day can help your intestinal cells and microbiome recover.
Glutamine is the first nutrient I recommend. It is the amino acid that feeds the small intestinal cells and helps your body to grow back a healthy intestinal lining. A high dose is not necessary even just 500 mg to 2000 mg per day makes a difference. You can get it as a single ingredient in a capsule or powder, or in a combination product with herbs that also help heal the gut lining.
That brings me to deglycyrrhizated herbal licorice , which is an anti-inflammatory herb known to help heal the intestines . I prefer it in powder form, but it is also available in capsules. I recommend it in combination with aloe vera, also known as an anti-inflammatory herb, which is extremely healing to digestion.
Fiber is a key substance that is absolutely needed for proper digestive health. Dozens of studies have linked IBS, or Irritable Bowel Syndrome, to lack of fiber in the diet. Some studies have also shown that when fiber is lacking, or over-consumed for that matter, there is a greater rate of SIBO, or Small Intestine Bacterial Overgrowth, as well as dysbiosis in general. Of course, both of these conditions connect back to leaky gut and an overgrowth of LPS. So its important to get enough, but not too much, of the best sources of both soluble and insoluble fiber, which come from whole foods.
How Do I Approach Gut Healing

The key to healing your gut is to first identify the primary drivers of your symptoms and then implement a methodical and systematic treatment approach. In treating patients clinically, the most common reasons for treatment failure involve either choosing the wrong therapy, choosing the wrong sequence or not giving a well chosen treatment enough time.
In most cases of gut dysfunction, we will first start with diet and lifestyle.We begin by removing anti-food and introduce nutrient-dense foods to support a more optimal gut microbiome. We seek to address the numerous stressors and environmental influences that can negatively impact our nervous system and hence our digestive function and gut motility. Optimizing sleep, spending time in nature and getting exercise can all positively improve aspects of gut function and the gut microbiome. In many cases, individuals can heal the gut simply from implementing rigorous dietary and lifestyle habits and will not require expensive supplement regimens.
If gut dysfunction persists despite making supportive dietary and lifestyle changes or an individual desires to accelerate healing, we can use a number of supportive therapies in sequence to improve gut health.
Typical supportive treatments in an example of a sequential order include:
Also Check: Is Peanut Butter Good For Gerd
Human Gut Tissue Sequence:
The primary goal of these very specialized segments of human gut tissue is to propagate ingested food and facilitate the digestion and absorption of key nutrients from the ingested food stuff. Beginning in the mouth, we start the initial digestion of certain carbohydrates as part of their passage into the stomach through the transport tube known as the esophagus. Once ingested food has made its way through the esophagus and into the stomach, we begin the formal digestion process with a substance known as hydrochloric acid or HCl. HCl functions primarily to denature certain proteins as well as to acidify the overall stomach contents as part of a non-specific antimicrobial response to various microorganisms. From the stomach, we move into the first segment of the small intestine, which is our primary tissue for the continued digestion and absorption of all the key macronutrients: carbohydrates, proteins and fats as well as our micronutrients: vitamins and minerals.
Allergies And Autoimmune Disease
Home Allergies and Autoimmune Disease
At first glance, allergies and diseases, such as rheumatoid arthritis, lupus and Hashimotos thyroiditis, may not seem like they have much in common. On one hand, our body is flagging harmless environmental allergens as dangerous and then going on the offense mode. While on the other hand, our immune system is attacking our own tissues. However, both are responses generated by the immune system, and that is where their similarities begin.
Allergies
Allergies involve an abnormal or hypersensitive reaction of the immune system when it encounters certain substances . The variety of symptoms produced can have an impact on quality of life and can even be life threatening in the case of anaphylaxis.1 Most allergies require long term management and are closely linked to asthma.
In 2017, 27.3% of Canadians aged 12 and older reported having allergies that had been diagnosed by allergy tests. Overall, females were slightly more likely to report having allergies than males . The respondents most commonly reported being allergic to pollens or grasses , followed by certain animals , dust mites and medications . Among allergy sufferers, roughly 43% reported being allergic to multiple allergens.2
Autoimmune Diseases
From the Microbiota to Superorganisms
Allergies and Autoimmune Diseases: Differences and Similarities
The Genetic Contribution
The GI Connection
The Leaky Gut Factor
Powerful Bacteria
The 5-R Program
References:
Recommended Reading: Sam E Side Effects Stomach Pain
Dr Fasano On Leaky Gut Syndrome And Gluten Sensitivity
Multiple research studies have linked gluten to the condition known as intestinal permeability AKA Leaky Gut Syndrome. I recently had the privilege of speaking with one of the leading gluten sensitivity researchers in the world, Dr. Alessio Fasano. He is the head of research at the University of Harvard Celiac Research Center, and he is responsible for discovering the gluten/leaky gut connection. In this video, we discuss how this condition can affect the gut, the brain, and multiple other tissues in the body
The Ultimate Support For Your Aip Journey
Get personalized guidance and support from Dr. Sarah in this 6-week interactive online course!
Thank you for your warmth, your AIP mastery, and your dedication to answering each and every one of our questions with such kindness and attention to detail. Thank you for teaching the science behind the principles. The amount of energy you put into creating this course and responding to us in real-time is felt and APPRECIATED!!-Nicole Wood
In fact, many studies have shown that increased intestinal permeability precedes the development of autoimmune disease . Yes, all the current science, including this new paper, show that a leaky gut comes first.
This is a quote from this new paper:
Recent observations in humans and in a variety of animal models indicate that an increased intestinal permeability , often referred to as a leaky gut, is playing a pathogenic role not only in development of gastrointestinal disorders like inflammatory bowel disease and celiac disease, but also in systemic autoimmune diseases, like type 1 diabetes .
What causes this leaky gut to develop? Well, until now, I and many others have postulated that this leaky gut can come from a variety of causes, from infection, to gut dysbiosis, to diet factors , to medications , to lifestyle factors . The mechanisms of how each of these can cause a leaky gut are well understood . But are these what cause the leaky gut in autoimmune disease? Maybe and maybe not.
You May Like: Will Turmeric Give You Diarrhea
Rise Of Autoimmune Disease Linked To Intestinal Permeability
Since the onset of World War II in 1939, autoimmune diseases have increased dramatically worldwide,1 encompassing more than 80 disorders.2 Collectively, autoimmune disorders are among the most prevalent diseases in the US they are the third most common category of disease after cancer and cardiovascular disease, affecting approximately 58% of the US population, or 14.7 to 23.5 million people.3 Statistics show that an estimated 78% of people with autoimmune conditions are women,3 and that these diseases are among the top 10 leading causes of death for girls and women of all age groups.1
Risk Factors
It is generally accepted that a common denominator in autoimmune disease is genetic susceptibility of the host immune system to misinterpret a benign environmental antigen as a threat.4 It is well known that the interaction between genes and the environment is fundamental to the immune response, but increasingly, research is validating a new paradigm in which genetic susceptibility coupled with increased intestinal permeability sets the stage for a specific environmental trigger. The trigger then causes a break in immunological tolerance and the onset of an autoimmune cascade.4
Mechanisms & Triggers
Certain aspects of gluten intake may influence the risk of CD occurrence: the amount of ingested gluten and the quality of ingested gluten.5 Recent studies also suggest that the pattern of infant nutrition may play a critical role in the development of CD.5
The Leaky Gut Diet Plan: What To Eat What To Avoid
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
The term leaky gut has gained a lot of attention in recent years.
Also known as increased intestinal permeability, its a condition in which gaps in your intestinal walls start to loosen. This makes it easier for larger substances, such as bacteria, toxins, and undigested food particles, to pass across the intestinal walls into your bloodstream.
Studies have associated increased intestinal permeability with several chronic and autoimmune diseases, including type 1 diabetes and celiac disease.
This article takes a close look at leaky gut and its causes. It also includes a list of foods that aid digestive health and a 1-week sample meal plan.
Read Also: How Long Does Ibs Flare Last
Gut Microbiota And Autism
2016 review , autistic children often develop significant digestive problems, such as constipation, diarrhea, and vomiting.
In a small 2017 study, researchers compared stool samples from two groups of children autistic children with GI symptoms, and those without autism or GI symptoms. The researchers identified significantly higher amounts of Clostridium perfringens bacteria in samples collected from autistic children with GI symptoms.
A Perfect Storm Of Perpetuating Imbalances Creates Autoimmunity
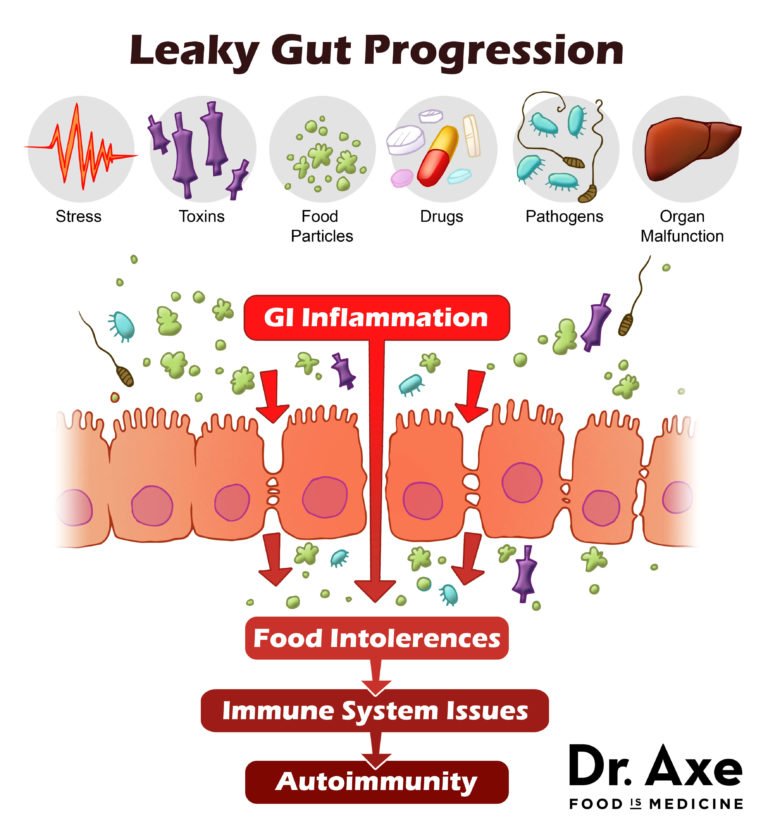
When an imbalance occurs in the microbiome, i.e. too few or too many of the right bacteria , too many of the wrong bacteria, or perhaps just the wrong kinds of bacteria in certain areas of the intestines, this increases the likelihood of triggering autoimmunity.
Thats because, in response to this imbalance, the signals to the immune system can shift, causing the immune system to become more inflammatory and start protecting us from our own cells. Autoimmunity can also be triggered by microbiome imbalance because this can encourage the growth of certain bacteria-produced toxins called Lipopolysaccharides . When certain bacteria overgrow, the level of LPS increases. LPS makes leaky gut worse and is associated with higher inflammation and more autoimmunity.
Why would dysregulation in the gut lead to issues with the immune system? The reason is simple. In the gut is where 80% of our immune system cells are located! The sheer volume of toxins produced by an overgrowth of pathogenic bacteria can begin to overwhelm the immune system as well as the systems of detoxification As a result, the immune system begins to react, sometimes in confused, sporadic, and irrational ways.
Unfortunately, over time, the cycle of Leaky Gut and autoimmunity can cause even more of a proliferation of imbalanced bacteria and more LPS overall, with heightened autoimmune disease symptoms and oxidative stress damaging cells and mitochondria.
Don’t Miss: Kidney And Stomach Pain Bloating
Making The Connection Gluten Free Societys Stance:
Most people assume that celiac disease and gluten sensitivity are the same thing. This archaic thought is rapidly changing. Although it is well established that gluten often impacts the villi of the small intestine, it has been shown to affect the body in a variety of other ways. These differences account for the massive failure of doctors to diagnose gluten sensitivity. Below is a diagram of environmental triggers to intestinal permeability . You will find that gluten sensitivity can directly and indirectly contribute to this problem. To the keen observer, this diagram illustrates why simple antibody testing fails to accurately diagnosis gluten sensitivity. Antibody production is only one lab component of a multi-faceted problem.
What The Medical Community Has To Say About Leaky Gut Syndrome
Do most conventional doctors support the idea that leaky gut is real?
WebMD refers to leaky gut as something of a medical mystery. This isnt surprising, since its not a diagnosis that most doctors have been taught in medical school. From an MDs standpoint, its a very gray area, says gastroenterologist Donald Kirby, MD Director of the Center for Human Nutrition at the Cleveland Clinic. In his opinion, Physicians dont know enough about the gut, which is our biggest immune system organ.
To make matters worse, government agencies have also contributed to the confusion. According to the United Kingdoms National Health Service , There is currently little evidence to support the theory that a porous bowel is the direct cause of any significant, widespread problems.
Yet, not everyone agrees. A roundtable review quotes the researchers at seven different European universities in 2014 agreeing upon the following:
Alteration of the gut barrier seems to have multiple consequences facilitating the onset of a variety of diseases depending on other hits and on genetic or epigenetic constellations, respectively. The growing significance of the gut barrier and bacterial translocation raises the questions of how we can improve gut barrier functions and gut microbiota.
So while its encouraging that science is coming around to leaky gut syndrome being a real problem, we are by no means at a point where there are standard diagnostic tools for testing and treating leaky gut.
You May Like: Pregnancy With Ibs
Final Thoughts On Gut Healing
Exploring gut healing can be intimidating! Using a framework that prioritizes diet and lifestyle and low risk supportive treatments will oftentimes lead to improved gut health for most patients. For those with autoimmune disease, focusing on the gut can lead to improved systemic symptoms and quality of life, and is far too often overlooked in favor of risky and more expensive treatments. If you feel stuck on how to get started or make progress, consider working with an integrative medicine provider who uses a simplified and iterative approach to addressing gut dysfunction. Additionally, my colleague and practice partner Dr. Michael Ruscio has some of the most evidenced based and accessible resources for gut health through his podcast, website and book.
May Reduce Inflammation And Symptoms Of Some Autoimmune Disorders
To date, the AIP diet has been tested in a small group of people and yielded seemingly positive results.
For instance, in a recent 11-week study in 15 people with IBD on an AIP diet, participants reported experiencing significantly fewer IBD-related symptoms by the end of the study. However, no significant changes in markers of inflammation were observed .
Similarly, a small study had people with IBD follow the AIP diet for 11 weeks. Participants reported significant improvements in bowel frequency, stress, and the ability to perform leisure or sport activities as early as 3 weeks into the study .
In another study, 16 women with Hashimotos thyroiditis, an autoimmune disorder affecting the thyroid gland, followed the AIP diet for 10 weeks. By the end of the study, inflammation and disease-related symptoms decreased by 29% and 68%, respectively.
Participants also reported significant improvements in their quality of life, despite there being no significant differences in their measures of thyroid function .
Although promising, studies remain small and few. Also, to date, they have only been performed on a small subset of people with autoimmune disorders. Therefore, more research is needed before strong conclusions can be made.
SUMMARY
The AIP diet may help reduce gut permeability and inflammation in people with autoimmune diseases. Small studies report beneficial effects in people with IBD and Hashimotos thyroiditis, but more research is needed to confirm these benefits.
Also Check: Ibs And Lettuce