Seek Professional Guidance For Ibs Associated With Bulimia
If you have been struggling with uncomfortable digestive symptoms that are a result of IBS while recovering from bulimia, it is crucial to seek out the appropriate help you need to allow your body to recover.
Minimizing eating disorder behaviors is a necessary step to avoiding further complications that may result from IBS. It is also important to work with your professional treatment team to understand how to best manage IBS while in recovery.
Your doctor may prescribe you certain medications and your registered dietitian may assist you with a meal plan to support your recovery efforts. Because of the complexity of having bulimia and IBS, professional guidance and treatment is a necessary component of healing and recovering from both of these disorders and their symptoms.
How To Handle Food Cravings When You Have Irritable Bowel Syndrome
Relief Report 023: Are you IBS Binge Eating?To get clear on your Triggers, download our checklist here https://stephanieclairmont.com/triggerchecklist
Posted by Stephanie Clairmont, RD on Wednesday, January 3, 2018
We all do it that afternoon snack attack when we get home after a long day. Once weve wrapped up whatever was keeping us busy all day, we often start to get the pre-dinner munchies. You know around 4-5pm every day when we start to crave a little something to eat. You might also be well aware that giving in to your craving for a little something can quickly spiral out of control, and before you know it, youve eaten so much that youre not even hungry once dinner finally gets on the table an hour later. I hate to be the one to tell you, but this habit is not always the best thing for us, especially when a lot of the foods we may choose to snack on could trigger our Irritable Bowel Syndrome symptoms. So how do we handle this binge eating with IBS?
How Disordered Eating Can Affect Your Gut
Pediatric gastroenterologist , has witnessed the damage that disordered eating can cause in patientseven in young children. He says that when a person restricts their food intake , the gut immediately suffers. We have two types of organs in our body: the vital organs and the non-vital organs, he says. Your heart, lungs, and kidneys are considered vital , while organs like those in the GI tract are considered less so. If you don’t give yourself the appropriate amount of calories, there will be a prioritization of nutrients, and they go to the vital organs first. Basically, severely restricting food starves your gut, which can lead to serious health problems.
Additionally, not eating enough food in general, or cutting way back on certain food groups, can disrupt your stomachs good bacteria, says Philadelphia-based registered dietitian Theresa Shank, RD. This bacterial imbalance can affect ones immune system and can contribute to symptoms of IBS or IBD.
According to Dr. Taño, behavior such as restricting or purging could lead to gastroparesis, where the stomach no longer properly contracts to break down food, delaying the digestive process. Gastroparesis can present itself as nausea or acid reflux after eating, or fullness well past a meal. Being malnourished can affect this, since your body is trying to preserve nutrients for more important functions, such as your circulatory system.
Recommended Reading: Ibs And Gastritis
Specific Concerns For The Ed Population
Traditionally, medical providers and dietitians have encouraged an elimination diet of some kind to treat these enduring and often puzzling symptoms. However, eliminating foods is really the opposite of the goal of nutrition therapy for EDs. Restriction, even if medically indicated, complicates ED recovery. In my personal experience, I have seen well-intended clients/practitioners advocate for an elimination protocol that has led to full blown relapse. So what are we to do as clinicians who feel desperate to help our clients fully recover and treat any concomitant digestive health concerns? I have a few take home points for you to consider.
What The Healing Process Is Like For The Gut
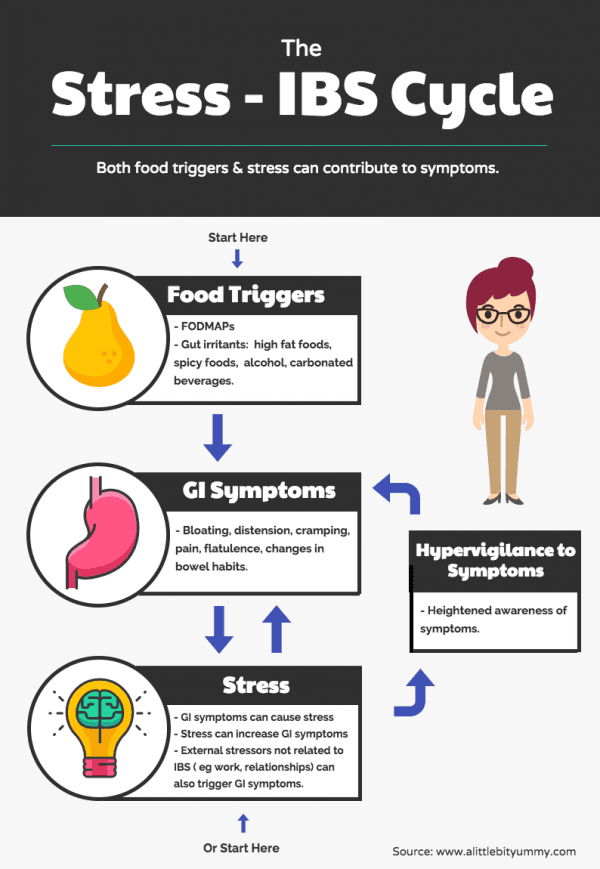
Additionally, many people with eating disorders experience IBS-type symptoms even as they begin the recovery process. When GI issues appear during recovery, anxiety and stress are often to blame. And in these cases, the symptoms can trigger disordered behaviors, such as restricting food in an attempt to soothe the distress.
It is quite common for a client to express that they feel better when they eliminate X, or X bothers their stomach so they avoid it. This often leads to veganism or a gluten- or sugar-free lifestyle,” says clinical psychologist Jaime Coffino, PhD, MPH. However, these decisions may be an extension of ones illness, and should only be made when fully recovered. Dr. Coffino often explains to clients, There will be many times throughout treatment that they do not feel good, or have anxiety. We explain that eating the food will help them get better, and avoiding the food will increase that anxiety.
The good news about digestive disorders associated with eating disorders is that they are often reversible. If you are navigating recovery and are concerned about your gut health, a certified eating disorder dietitian or a primary care doctor knowledgeable about eating disorders should be your first stop, not an influencer pushing Whole30. For me, eliminating foods was not the solution to fixing my gut health issues. It took working with professionals to manage my anxiety and get back to eating foods that I enjoy, and my gut has thanked me for that.
Don’t Miss: Does Peppermint Tea Help With Constipation
The One Thing I’m Realizing Two Years After My Eating Disorder
When I was in the deepest, darkest depths of my orthorexia, I had one fear that overwhelmed all of the others. Food. Not all food, but certainly most foods.
While other young girls my age where enamored with boys, I was concerned with sandwiches. While other students in my college classes were going to happy hours, I was going to the gym and then straight home to bulk cook my specially prepared salt-less, fat-less, yummy-less meals.
I was obsessed with not only eating clean and pure foods at all times of the day, but I was also obsessed with living an entire lifestyle that revolved around appearing healthy. Every semi-enjoyable activity I did was scheduled around how hard I workout out earlier, how many calories I burned, how many I ate, and how good I was at eating the standards I set for myself.
That was my life for about five years. It’s been two years since those days and I’m fortunate to be able to say that I experience freedom with my food choices today, as well as how I move my body. I’ve said goodbye to being chained by a “perfect” body and instead, I live my intuition-driven life exactly how I want, which has led to so many fulfilling side effects.
One side effect I did not expect has been creeping up on me lately. Since I began eating disorder recovery, I have been slowly eating all of the foods that once terrified me. It was so liberating. I could drink lattes, eat burritos, have pizza, salads with numerous ingredients and unlimited amounts of fruit!
Training Program For Clinicians
If you want to bring more to your clients with digestive issues, Lauren Dear and I have teamed up and developed an online training to build your confidence working with those challenging clients who have eating disorders and digestive disorders.
Selected Citations
Abraham, S., & Kellow, J. . Exploring eating disorder quality of life and functional gastrointestinal disorders among eating disorder patients. Journal of Psychosomatic Research, 70, 372377.Boyd, C., Abraham, S., & Kellow, J. . Appearance and disappearance of functional gastrointestinal disorders in patients with eating disorders. Neurogastroenterology and Motility, 22, 12791283.Kleiman, S. C., Watson, H. J., Bulik-Sullivan, E. C., Huh, E. Y., Tarantino, L. M., Bulik, C. M., & Carroll, I. M. . The Intestinal Microbiota in Acute Anorexia Nervosa and During Renourishment: Relationship to Depression, Anxiety, and Eating Disorder Psychopathology. Psychosomatic Medicine, 77, 969981. Peters, SL. . Randomised clinical trial: the efficacy of gut-directed hypnotherapy is similar to that of the low FODMAP diet for the treatment of irritable bowel syndrome. Aliment Pharmacol Ther. Sep 44:447-59. Sato, Y., & Fukuco S. . Gastrointestinal symptoms and disorders in patients with eating disorders. Clin J Gastroenterol, Oct 8:255-63. Surdea-Blaga, T., Baban, A., Nedelcu, L., Dumitrascu, D. . Psychological interventions for irritable bowel syndrome. Journal of Gastrointestinal and Liver Diseases, 25.
Read Also: Food Poisoning Constipation
Eating Disorders Can Also Give Rise To Gut Issues
Individuals who suffer from eating disorders such as anorexia nervosa , bulimia nervosa , binge eating disorder or avoidant/restrictive food intake disorder tend to suffer from myriad psychological symptoms such as anxiety and depression, in addition to disordered eating behaviors and rigid thought patterns.
Here again, we see the effects of anxiety on gut function, whereby during especially high stress periods, individuals with eating disorders may experience significant gut distress in the form of cramping, pain, bloating, diarrhea and/or constipation.
Additionally, certain disordered eating patterns can have a direct and unpleasant effect on digestion and overall gut function. For example, individuals with BN or BED may eat extremely large quantities of food in one sitting, which can stretch the stomachs capacity and lead to bloating, pain or cramping.
Individuals with BN who frequently purge put severe stress on their entire GI tract, which can cause stomach damage or rupture, esophageal damage and/or chronic GERD , and imbalance of important electrolytes, which can also further exacerbate gut issues.
Finally, those with AN may find that their entire GI tract begins to slow due to lack of food intake, leading to delayed gastric emptying, gastroparesis, and/or constipation, with accompanying symptoms of early satiety, nausea, vomiting and/or bloating.
You may want to read: GERD, IBS & The Low FODMAP Diet
Slow Gastric Motility And Functional Dyspepsia
As mentioned earlier, patients with eating disorders frequently report postprandial fullness, abdominal distention, gastric distension, early satiety, and nausea . Both AN and BN patients have reported more severe postprandial distress than healthy controls . These symptoms may be attributed to postprandial distress syndrome, a subtype of functional dyspepsia. Functional dyspepsia, itself a type of FGID, manifests as postprandial fullness, early satiation, epigastric pain, or epigastric burning without any structural disease . In patients with eating disorders, one study reported a prevalence rate of 45 % for postprandial distress syndrome , and another study reported a prevelance rate of 23 % for functional dyspepsia .
Slow gastric motility contributes to these gastric symptoms. AN patients have shown slow gastric emptying in addition to gastric dysrhythmia, impaired antral contractility, delayed emptying of solids, decreased postcibal blood levels of norepinephrine and neurotensin, and impaired autonomic function . Slow gastric emptying in these patients was found to correlate with nausea, vomiting, and gastric fullness , and has the potential to lead to difficulties during re-feeding and weight restoration .
In BN patients, gastric relaxation after food intake was significantly diminished , although gastric emptying was normal . Gastric compliance in BN showed no difference from that in controls .
Read Also: Side Effects Of Sodium Bicarbonate
Ibs Diet: What To Do And What To Avoid
The influence of diet is unique to each person. There is no generalized dietary advice that will work for everyone.
A healthcare provider can take a brief dietary history and help identify dietary and/or other factors that may impact symptoms. Keeping a diary for 23 weeks of dietary intake, symptoms, and any associated factors can help with this.
For those with irritable bowel syndrome who benefit from simple dietary modifications, it makes sense to adjust the diet and reduce the intake of the offending food. It does not make sense to adopt unnecessarily limited diets. This can lead to reduced quality of life or even malnutrition.
Healthcare providers and patients need to talk about diet. Guidance needs to be provided by a knowledgeable health care professional . They can assess individual circumstances affecting IBS, while helping make sure that nutritional needs are being met through a balanced diet, and healthy eating habits.
What Is The Link Between Ibs And Eating Disorders
Studies have found that gastrointestinal consequences are seen in people suffering from eating disorders, the most common of which being IBS. Present evidence suggests that IBS usually appears after the development of an eating disorder.
The link between IBS and Eating Disorders
IBS symptoms and gut dysfunction have been observed mostly in people with anorexia and bulimia, as a result of malnutrition, nutrient deficiency, and alternating between binging and self-induced vomiting. Psychological problems usually accompanying eating disorders, such as anxiety and obsessive-compulsive features, can worsen the severity of symptoms resulting in long lasting IBS.
The development of IBS in people suffering from eating disorders may delay their recovery from the illness, causing trouble with weight restoration and re-feeding, thus leading to the persistence of the disordered behaviour. IBS may exacerbate the fear of eating certain foods due to the physical discomfort that individuals experience following a meal.
Bloating is often confused with the experience of feeling fat in eating disorders and can be a major obstacle to recovery.
Read Also: Colostrum To Heal Leaky Gut
Pain Unrelated To Bowel Movements
In people with IBS, the criteria for diagnosis says abdominal pain should be related to bowel movements.
Many IBS patients say this is not always true. But for the most part, people with IBS feel like their pain has something to do with their diarrhea or constipation.
If you have pain you don’t think is related to your bowel movements, talk to your doctor. It may still be IBS, but it is worth looking at other possibilities.
If you have an IBS diagnosis but you think your pain is not typical of IBS, talk to your doctor at once. Persistent pain should always be evaluated by a doctor.
Cdhf Talks: Ibs And The Gut Microbiome
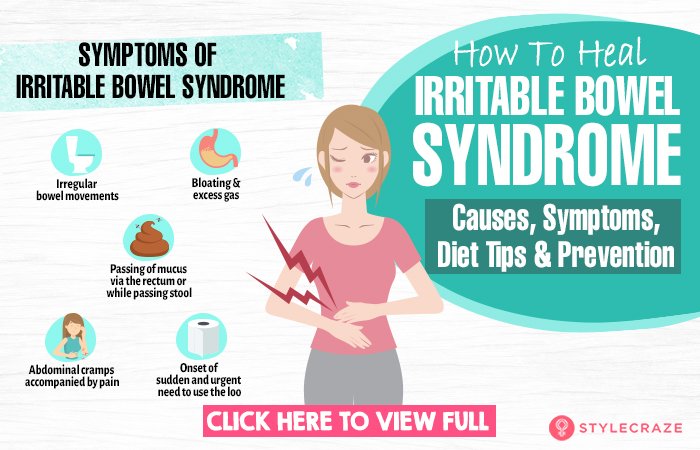
We are very excited to announce our new #CDHFTalks with Dr. Turbide, gastroenterologist at the University of Calgary on a digestive condition that you may be familiar with – Irritable Bowel Syndrome, or IBS for short. IBS is a chronic pain disorder, that is very common within the Canadian Population.
In this series of videos, Dr. Turbide goes over all things IBS what it is, the different types of IBS, if your microbiome can be a cause of your IBS, and tips on managing IBS. He also talks about all of the treatment options available – whether that be prescription medications, over-the-counter medications, or psycho-social interventions.
This is one you definitely dont want to miss so have a watch here.
Recommended Reading: Acid Reflux Headache Remedies
Where Do These Problems Come From How Do I Maintain A Healthy Diet
It is important to be aware of your family history regarding food allergies and intolerances allergies, in particular, can run in families. Monitor what children eat and gauge their physical reactions to new foods since most food allergies develop in childhood. If you suspect a food allergy, a visit to an allergist can help determine which particular foods you may have immune reactions to. A healthy diet can still be maintained if someone has a food intolerance or a limited number of allergies. Still, individuals with complex allergies and severe reactions should work with a registered dietician to ensure that they consume the macro and micronutrients they need while avoiding the allergens.
For further information about food allergies, visit .
Resources for Phoenix-area families can be found at .
Superior Mesenteric Artery Syndrome
Superior mesenteric artery syndrome is the result of compression of the third portion of the duodenum, which lies between the aorta and the vertebral column posteriorly and the superior mesenteric artery anteriorly . In healthy individuals, the arch of the SMA is held away from the aorta by the mesenteric pad of fat. Considerable loss of mesenteric fat in conditions such as burns, prolonged bedrest, rapid growth in children without corresponding weight gain, and AN, serves to reduce the aortomesenteric angle . Weight loss is regarded to be a risk factor for SMA syndrome . The symptoms of the syndrome are appetite loss, abdominal pain, postprandial distension, abdominal fullness, nausea, and vomiting .
Radiological methods are useful for diagnosing SMA syndrome. Barium swallow radiography demonstrates an extremely dilated stomach and restriction of contrast flow past the third portion of the duodenum . Computed tomography reveals dilation of the stomach and proximal duodenum in addition to severe narrowing of the third portion of the duodenum . Contrast-enhanced CT reveals compression of the duodenum between the SMA and aorta .
BN patients rarely develop SMA syndrome because of their normal body weight. Ikegaya et al. reported a fatal case of BN in a woman who consumed enormous amounts of solid food, where her distended stomach compressed the SMA and pinched the duodenum, eventually leading to fatal total intestinal obstruction .
Also Check: Ergotamine In Pregnancy
Treating Irritable Bowel Syndrome With Constipation
It isimportant to find a solution that works best for you so you can find relief andenjoy the best quality of life possible despite IBS-C. Your healthcare providerwill try to help you manage your symptoms. Recommendations generally begin withchanges to lifestyle and diet. If those changes do not bring relief,over-the-counter products or prescription medications may be prescribed.
Support Our Nonprofit Magazine
Before you start reading…There has never been a time when our community and content was needed more. Unlike other sites, we don’t publish sponsored content or share affiliate links. We also dont run ads on our site and dont have any paywalls in front of our content-anyone can access all of it for free.
This means we rely on donations from our community to keep our site running. We want to be here to support you all through this pandemic and beyond, which is why we are asking you to consider donating whatever you are able.
A single donation of just $5 will make a HUGE difference and will help keep our nonprofit running so we can continue offering peer support for mental health through our content.
Also Check: Pancreatitis And Probiotics