Symptoms Of Diverticular Disease
Please pay close attention to the use of the similar but distinctly different definitions: the condition of diverticular disease and inflammation of the diverticula .
Diverticulosis is often present without any symptoms. Many symptoms are similar to those of irritable bowel syndrome and often include changing bowel activities such as constipation, diarrhea, or alternating between the two extreme stool consistencies.
Diverticulitis occurs when the diverticula become inflamed and/or infected. There might be an increase in diarrhea, cramping, and bowel irritability, and symptoms can include intense pain, abdominal cramping, bleeding, bloating, and fever. The pain and tenderness is often in the left lower portion of the abdomen.
Rarely, fistulae, bowel obstruction, and lower intestinal hemorrhage occur, or a diverticulum can perforate, causing a local abscess with a marked increase in the degree and nature of the pain. Additional symptoms are likely to include fever, nausea, and vomiting. Sometimes these complications require urgent surgery.
Diagnosing Diverticular Disease And Diverticulitis
Diverticular disease can be difficult to diagnose from the symptoms, alone because there are other conditions that cause similar symptoms, such as irritable bowel syndrome .
As a first step, your GP may recommend blood tests to rule out other conditions such as coeliac disease or bowel cancer.
In some cases, you may be offered treatment for IBS and diverticular disease at the same time.
What Is Diverticulosis And Diverticulitis
Diverticulosis: Diverticulosis is the condition of having small pouches protruding from the wall of the colon. These pouches are extremely common among Americans, for example, where about 1 out of 10 people over age 40, half of those older than 60, and 2 out of 3 over age 80 have them.
Diverticulosis itself is really not a problem, as the pouches themselves are harmless and rarely cause symptoms. However, the situation becomes more serious if the pouches become infected from, for example, stool getting trapped in the pouch.
Diverticulitis: If infection occurs, the condition is called diverticulitis. Diverticulitis is more serious because infection can lead to other problems. Diverticulosis leads to diverticulitis in about 1 out of 5 to 1 out of 7 cases.
Researchers think a diet low in fiber is to blame for a high incidence of diverticulosis. Fiber is important because it helps keep stool soft and bulky so it can pass easily through the colon. Without enough fiber stool becomes hard, which creates pressure in the colon as the muscles strain to move the stool. This pressure is what causes the parts of the wall of the colon to pop out into pouches.
Don’t Miss: What Fruit Is Good For Diarrhea
Dietary Treatments For Ibs
For many people with IBS, diet can play a significant role. Your doctor or nutritionist may recommend avoiding certain foods to help you avoid triggering symptoms of IBS. One group of foods your doctor may recommend are those containing high levels of FODMAPs. FODMAPs are short-chain carbohydrates found in many grains, fruits and vegetables that have been shown to worsen IBS symptoms. The low-FODMAP diet involves removing these foods, and was developed by Monash University to treat symptoms of IBS.
Evaluation Of The Ibs Cohort For Misdiagnosis And Diverticulosis Documentation
Two gastroenterologists independently reviewed the medical records of patients in the IBS cohort who had an initial episode of outpatient clinically diagnosed, antibiotic-treated diverticulitis. They recorded data from the outpatient visits when the diagnoses were made, including clinical features and leukocyte counts. Fever was defined as temperature > 37.5°C and leukocytosis as > 11,500 leukocytes/mm3. They searched outpatient visit records, hospitalization summaries, and laboratory and pathology reports following the visit for evidence of a revised diagnosis with changed therapy or exclusion of diverticulitis, the latter requiring CT 3 days after diagnosis that revealed no colonic wall thickening, inflammation of peri-colic fat, or other findings of diverticulitis. They recorded all barium enema, flexible sigmoidoscopy, colonoscopy, and abdominopelvic CT procedures performed before and after the diagnosis and considered the patient as having diverticulosis if a single procedure reported diverticulosis of any severity. Patients with multiple imaging tests were classified as having no diverticulosis only if no procedure reported it, either before or after the diagnosis. The reviewers resolved any discrepancies by joint record review.
Also Check: When Do Ib Scores Come Out
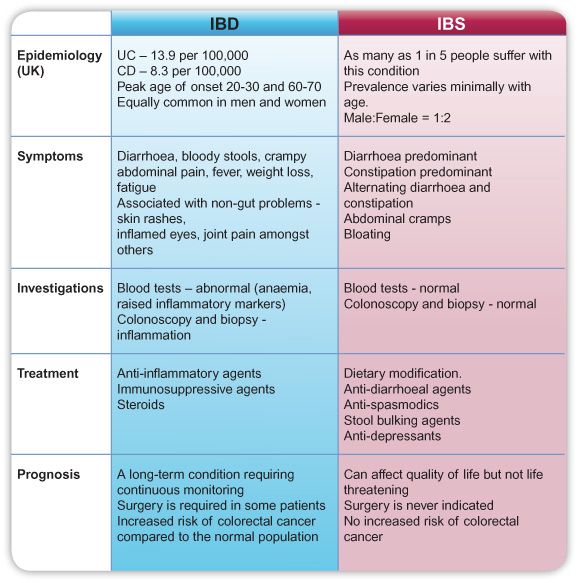
Comparing Diverticulitis And Irritable Bowel Syndrome Signs And Symptoms
Signs and symptoms of diverticulitis include severe pain in the lower left side of the abdomen , nausea and vomiting, fever, abdominal tenderness, constipation, and in some cases diarrhea .
The muscles in the colon of an IBS patient contract more readily than in normal people, leading to the various symptoms including:
- Diarrhea, constipation, or alternating between the two
- Abdominal pains or cramps
- Bowel movements that are harder or looser than usual
How Is Diverticular Disease Diagnosed
Diagnosis is made by examination of the inside of the colon. During the examination the doctor or nurse endoscopist will be looking for other abnormalities that could be causing your symptoms and so diagnosis is only confirmed once other conditions have been ruled out. This can be done via: Colonoscopy or sigmoidoscopy. A tube with a camera is passed into the colon via the back passage to view the inner surface of the colon. A sigmoidoscopy is a similar procedure that views less of the colon. Medication can be given to make the procedure comfortable and you will be given something before the procedure to ensure you completely empty your bowels. CT scan. This is a non-invasive x-ray-based test although, as with the colonoscopy, you will be required to completely empty your bowels beforehand.
Don’t Miss: Can An Enlarged Prostate Cause Constipation
Possible Connection Between Ibs And Diverticulosis
There may be a connection between IBS and diverticulosis.
One 2013 study followed over one thousand people who were diagnosed with diverticulitis, with no previous history of a functional gastrointestinal disorder , such as IBS, over a period of approximately six years. Compared with a control group, they found that these individuals were at an almost five times greater risk for developing IBS. These results led this group of researchers to propose the notion of “post-diverticulitis IBS” , though it is not yet considered an official sub-type of IBS.
Other researchers have concluded that a link may exist, but that the connection and its implications for treatment are not yet clear.
Diverticular Disease And Diverticulitis
Diverticular disease and diverticulitis are related digestive conditions that affect the large intestine .
Diverticula are small bulges or pockets that can develop in the lining of the intestine as you get older.
Most people with diverticula do not get any symptoms and only know they have them after having a scan for another reason.
When there are no symptoms, it is called diverticulosis.
When diverticula cause symptoms, such as pain in the lower tummy, it’s called diverticular disease.
If the diverticula become inflamed or infected, causing more severe symptoms, it’s called diverticulitis.
You’re more likely to get diverticular disease and diverticulitis if you do not get enough fibre in your diet.
Also Check: Is Apple Cider Vinegar A Prebiotic Or A Probiotic
What Causes Diverticulitis And Diverticulosis
Experts dont know for sure what causes these conditions, but several factors may play a role:
- High pressure in the colon: Muscle spasms in the colon or straining to have a bowel movement may cause bulges to form at weak spots.
- Family history: The genes you inherit may make you more likely to develop diverticulosis and diverticulitis.
- Medications: Studies have uncovered connections between these digestive conditions and some medicines, including nonsteroidal anti-inflammatory drugs like aspirin.
- Lifestyle: Lack of exercise, obesity and smoking may also contribute.
Dr. Fayez Abboud talks about what causes diverticulitis.
Click play to watch the video or read video transcript.
What causes diverticulitis?
How Do Ibs And Diverticulitis Differ
IBS is a common gastrointestinal disease. Its characterized by abdominal pain and changes in the frequency and quality of your bowel movements. Symptoms tend to flare up periodically.
How IBS develops still is not well understood. But its been linked to:
- food passing through your gut too quickly or slowly
- an oversensitivity of the nerves in your gut
Diverticulitis is a condition that develops in your large intestine . Its caused by an infection in a diverticulum, which is a weakened area of your colon wall that can bulge out and form a pocket or pouch. Diverticula can range from pea-size to much larger pockets.
Diverticulitis develops when one of these pockets becomes inflamed and infected by bacteria in stool that gets pushed into the diverticula. You may feel pain in your abdomen and may also feel nauseous and feverish.
People with diverticulitis in Western societies, such as the United States or Europe, are much more likely to develop diverticula on their left side. But people of Asian descent are more likely to develop diverticula on their right side.
You May Like: Why Does My Stomach Feel Tight And Bloated
Diverticulitis Diet Foods To Avoid #: Certain Fruits
Certain fruits like apples, pears and plums should be avoided with diverticulitis. These foods are also high FODMAP foods but for a different reason. These fruits are high in fructose, a naturally occurring sugar in fruits. If you have diverticulitis, and eat too much fructose, it could contribute to sugar fermentation in your gut and therefore to the symptoms of diverticulitis.
Dietary Tips For Ibs And Diverticulitis

You may be able to relieve your IBS symptoms by:
- eating no more than 3 portions of fresh fruit per day
- drinking no more than 3 cups of tea or coffee per day
- following a low FODMAP diet
- eating your food slowly
- cooking most of your meals at home using fresh ingredients
You may be able to ease diverticulitis symptoms by:
- following a liquid diet until pain subsides
- adding more high fiber foods to your diet
- avoiding foods that seem to trigger your symptoms
You May Like: Can Hemorrhoids Cause Abdominal Pain And Bloating
Diverticulitis Vs Irritable Bowel Syndrome: Risk Factors And Complications
Risk factors that can increase a persons risk of developing diverticulitis include older age, obesity, smoking, lack of exercise, diet high in animal fat and low in fiber, and certain medications.
Complications that can arise from diverticulitis include the development of an abscess, a blockage of the colon or small intestine, the formation of fistulas, and peritonitis if the inflamed pouches rupture spilling intestinal contents into the abdomen.
You are more likely to have IBS if you are:
- Under the age of 45
- Related to an IBS patient
- Suffering a mental health problem .
IBS complications include diarrhea or constipation, aggravating hemorrhoids, and intolerance to certain foods. IBS may cause you to have a reduced quality of life as you must be mindful of what you eat, which could lead to depression. Make sure to take care of your mental health if youre living with IBS, as mental problems could worsen your condition.
Ct Pneumocolon Or Colonography
Another technique for confirming the presence of diverticula is a computerised tomography . A CT scan uses X-rays and a computer to create detailed images of the inside of the body.
As with a colonoscopy, you will be given a laxative to clear out your bowels before you have the CT scan.
Unlike a regular CT scan, the colonography scan involves a tube being inserted into your rectum, which is used to pump some air up into your rectum. The CT scan is then taken with you lying on your front, and again lying on your back.
You may need to have an injection of contrast dye before the scan, but this is not always necessary.
You May Like: Does Black Tea Cause Constipation
What Are The Best Probiotics For Ibs And Diverticulitis
There are literally hundreds of different kinds of bacteria that live in your digestive tract, and therefore hundreds of different kinds of probiotics. The best probiotics for treating IBS and diverticulitis will vary based on the individual needs of the patient. This must be properly assessed before any recommendation can be made on which probiotics are best for that patient.
Ready to Treat Your DiverticulitisSuccessfully treating diverticulitis remains a key component of what we do at the IBS Treatment Center and is very similar to our approach to IBS. To learn more about our approach, please give us a call 888-546-6283 at or schedule an appointment with us. We have a telemedicine option so there is no need to come to our office in person.
Can Ibs Lead To Diverticulitis
There is no medical evidence that suggests that IBS leads to diverticulitis. However, this IBS diverticular disease research study proved, people with IBS have a significantly increased risk for developing diverticulosis. This explains why people can have both IBS and diverticulitis, and why they often get them confused.
Recommended Reading: How To Change Gut Microbiome To Lose Weight
Diverticulitis Diagnosis Frequency And Associations In Ibs And Non
Of 89,008 examinees, we excluded 21,181 as detailed in , yielding 67,827 examinees, 3836 IBS and 63,991 non-IBS examinees. Additional exclusions by electronic database criteria yielded 290 IBS individuals with 523 episodes and 1669 non-IBS individuals with 2455 episodes.
Twelve Patients with Irritable Bowel Syndrome Whose Diagnosis of Diverticulitis Was Subsequently Revised or Excluded
Twenty-nine patients had no diagnosis revision, but they had colon imaging that did not reveal diverticulosis before and/or after diagnosis. As detailed in , the age of these patients ranged from 25 to 84 years, 26 were female, and at least 1 procedure revealing no diverticulosis occurred before, after or both before and after diagnosis in 5, 15, and 9 patients, respectively. Nineteen patients had > 1 negative procedure, including 11 who underwent 3 procedures.
Combined with the revised diagnoses or CT exclusion of diverticulitis in 12 patients, a lack of diverticulosis on imaging supported misdiagnosis in 41 of 189 patients. One hundred forty-two patients had a diagnosis that was not revised nor excluded by CT and had imaging before and/or after the episode that revealed diverticulosis. Six had no colon imaging.
Differentiating Diverticulitis And Irritable Bowel Syndrome Treatment
Medical treatments for diverticulitis include antibiotics to treat infection, liquid diet to allow bowels to heal, and over-the-counter pain relievers. In complicated cases of diverticulitis, surgery may be required, such as primary bowel resection, where the affected part of the intestine is removed and the rest of it is reconnected. Another option is bowel resection with colostomy if it is impossible to reconnect the colon to the rectum due to inflammation.
If diverticulitis is causing pain, there are home remedies you can try for relief. To reduce muscle cramping caused by diverticulitis, you can apply heat to the abdomen. Meditation, too, may be beneficial for pain management. If you still need to opt for a pain reliever, stay away from ibuprofen and reach for acetaminophen instead.
There are also some preventative measures you can try to lower your risk of developing diverticulitis.
Regular exercise, in particular, is beneficial for diverticulitis prevention, because it helps keep bowels regular and reduce pressure on the colon. Added pressure can result in the formation of diverticula.
Fiber is essential for bowel regularity, too. And, in this vein, staying hydrated helps. Although fiber can help you stay regular, without enough fluids it can have the opposite effect. Staying hydrated improves bodily functions, so its important to drink enough water.
Dietary changes:
Recommended Reading: Can A Herniated Disc Cause Constipation
The Ibs Diet: A Guide To Getting Started
To understand what to eat with irritable bowel syndrome , it is helpful to understand a few key things about it. IBS is a gut-brain disorder, which means the problem arises from the way the brain and the gut work together. The sensitivities that occur with IBS result from the way the muscles in the gut contract. With IBS, there is often no sign of visible damage or disease in the bowel.
Treating Diverticular Disease And Diverticulitis
A high-fibre diet can often ease symptoms of diverticular disease, and paracetamol can be used to relieve pain other painkillers such as aspirin or ibuprofen are not recommended for regular use, as they can cause stomach upsets. Speak to your GP if paracetamol alone is not working.
Mild diverticulitis can usually be treated at home with antibiotics prescribed by your GP. More serious cases may need hospital treatment to prevent and treat complications.
Surgery to remove the affected section of the intestine is sometimes recommended if there have been serious complications, although this is rare.
Don’t Miss: Is Granola Ok For Ibs
How Are Diverticulitis And Diverticulosis Treated
Diverticulosis: With the goal of preventing bothersome symptoms or more serious problems like diverticulitis, these can help:
- High-fiber diet: Foods rich in fiber can help you avoid symptoms if you already have the condition. Increase fiber in your diet slowly to decrease the chances of abdominal gas and pain.
- Medicines: Mesalazine and the antibiotic rifaximin may help reduce symptoms.
- Probiotics: Probiotics are healthy bacteria, like those that naturally live in your stomach and intestines. You can find them in dietary supplements and in foods like yogurt. Talk with your doctor or health care provider first about using these or any alternative medicines.
Diverticulitis: Treatment will depend on your symptoms.
- Mild symptoms: You may be put on a liquid diet for a short time. Antibiotics are often prescribed. If these help, your doctor may put you on a high-fiber diet.
- Severe symptoms: You may be admitted to the hospital, where you can be given intravenous antibiotics and fluids. You will also be put on a low-fiber or liquid diet. In rare cases, surgery may be needed.
What Is Diverticular Disease
- Diverticulosis is a condition that describes small pouches in the wall of the digestive tract that occurs when the inner layer of the digestive tract bulges through weak spots in the outer layer. When these diverticula become inflamed, that is called diverticulitis.
- One of the main causes of diverticulosis is a diet low in fiber.
- Many people with diverticulosis have no symptoms. When symptoms do occur they can include:
- Pain in the abdomen
Recommended Reading: Can Almond Milk Cause Constipation